Key Takeaway
Umbrella review of 17 meta-analyses (68 RCTs) found high-quality evidence for reduced triglycerides and seizure frequency, but also raised LDL cholesterol — a clinically meaningful concern.
Summary
This umbrella review — the highest level of evidence synthesis — examined 17 meta-analyses comprising 68 RCTs across 115 health associations for ketogenic diets. It graded evidence quality for each outcome.
High-quality evidence (4 associations) supported reduced triglycerides, decreased seizure frequency, and reduced seizure severity, but also elevated LDL cholesterol. Moderate-quality evidence (4 associations) supported body weight reduction, lower HbA1c, decreased respiratory exchange ratio, and elevated total cholesterol. The remaining 43 significant associations were supported by low-to-very-low quality evidence.
Very low-calorie ketogenic diets improved body composition without worsening muscle mass, but standard ketogenic low-carb high-fat diets reduced muscle mass in healthy populations. The authors recommend long-term follow-up trials to determine whether short-term metabolic improvements translate to reduced cardiovascular events and mortality.
Methods
- Umbrella review of 17 meta-analyses (68 RCTs)
- 115 unique health associations analyzed
- Three diet types: KD, ketogenic LCHF, very low-calorie KD
- Evidence graded by quality (high, moderate, low, very low)
Key Results
- High-quality: reduced triglycerides, reduced seizures, but increased LDL
- Moderate-quality: weight loss, lower HbA1c, increased total cholesterol
- VLCKD preserved muscle mass; standard K-LCHF reduced muscle mass
- 51 of 115 associations statistically significant
Figures
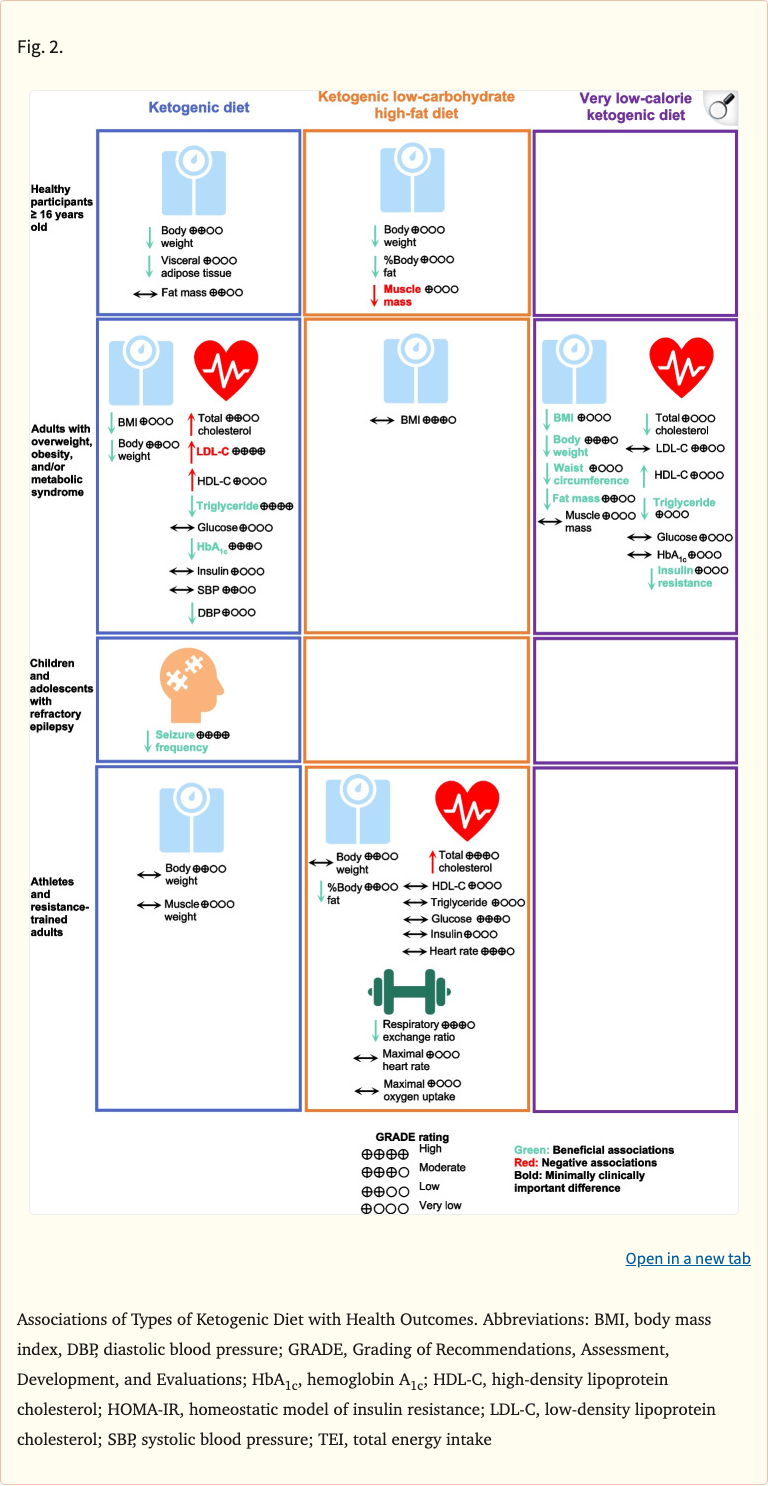 Figure 1
Figure 1
Limitations
- Most evidence was low-to-very-low quality (43/51 significant associations)
- Long-term effects beyond 12 months poorly studied
- LDL increase raises cardiovascular safety questions
