Key Takeaway
Qigong therapy significantly reduces depression severity in adults with major depressive disorder, with a moderate-to-large effect size (Hedges' g = -0.64) compared to both active and passive controls.
Summary
This meta-analysis examined the effectiveness of qigong-based therapy for adults diagnosed with major depressive disorder (MDD). The review searched six electronic databases for randomized controlled trials comparing qigong interventions to control conditions.
The pooled analysis found that qigong-based therapy produced a significant reduction in depression severity with a moderate-to-large effect size (Hedges' g = -0.64, 95% CI -0.92 to -0.35, p < 0.001). Heterogeneity was moderate (I-squared = 41.73%), suggesting reasonably consistent results across studies.
Notably, qigong was effective compared to both active controls such as exercise or cognitive-behavioral therapy (Hedges' g = -0.47) and passive controls such as waitlist or usual care (Hedges' g = -0.80). The larger effect against passive controls is expected, but the significant effect against active controls is particularly meaningful, suggesting qigong offers unique therapeutic benefits beyond general physical activity.
The findings support qigong as a viable complementary treatment option for adults with MDD, particularly for those who may not respond well to conventional treatments or prefer mind-body approaches.
Methods
- Systematic search across six electronic databases
- Included only RCTs with MDD-diagnosed participants
- Subgroup analysis by control type (active vs passive)
- Effect sizes calculated using Hedges' g
- Heterogeneity assessed with I-squared statistic
- Publication bias evaluated with funnel plots
Key Results
- Overall effect: Hedges' g = -0.64 (95% CI -0.92 to -0.35, p < 0.001)
- Effect vs active controls: Hedges' g = -0.47 (significant)
- Effect vs passive controls: Hedges' g = -0.80 (significant)
- Moderate heterogeneity (I-squared = 41.73%)
- Qigong outperformed both exercise and waitlist conditions
Figures
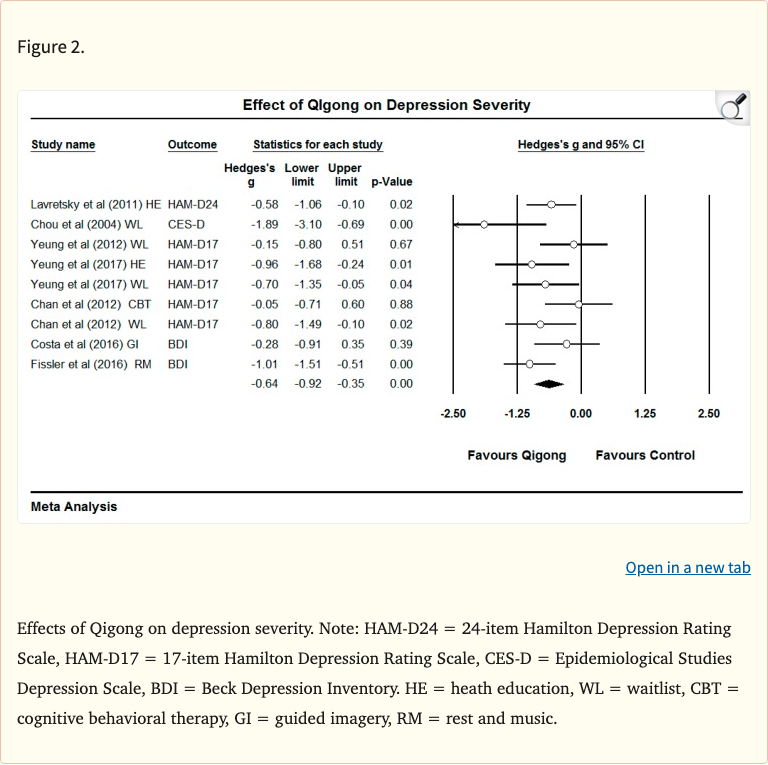 Figure 1
Figure 1
Limitations
- Limited number of eligible RCTs
- Most studies from Chinese populations
- Variable qigong styles and intervention durations
- Some studies had small sample sizes
- Blinding difficult in mind-body intervention trials
- Long-term follow-up data limited
