Key Takeaway
Relaxation therapy (primarily PMR) significantly reduced post-operative pain scores (WMD -1.27 on VAS) and anxiety in abdominal surgery patients across 11 RCTs.
Summary
This systematic review and meta-analysis examined the efficacy of relaxation therapy, primarily progressive muscle relaxation, as a nursing intervention for post-operative pain relief in patients undergoing abdominal surgery. The authors searched PubMed, Embase, Cochrane Library, and Web of Science for randomized controlled trials.
Eleven RCTs were included in the analysis. The pooled results showed that relaxation therapy significantly reduced post-operative pain intensity as measured by the Visual Analog Scale (WMD -1.27, 95% CI: -1.94 to -0.60, p < 0.001). The intervention also significantly reduced anxiety levels and decreased analgesic consumption compared to standard care. Subgroup analysis indicated that progressive muscle relaxation was the most commonly studied and effective technique.
The findings support the integration of relaxation therapy, particularly PMR, into post-operative nursing care for abdominal surgery patients. As a non-pharmacological, cost-free intervention with no side effects, it provides a valuable complement to standard pain management protocols and can reduce reliance on opioid analgesics.
Methods
Systematic review and meta-analysis following PRISMA guidelines. Searched PubMed, Embase, Cochrane Library, and Web of Science for RCTs of relaxation therapy in post-operative abdominal surgery patients. Included 11 RCTs. Quality assessed using the Cochrane risk of bias tool. Weighted mean differences (WMD) calculated using random-effects models. Pain measured primarily using the Visual Analog Scale (VAS).
Key Results
Relaxation therapy significantly reduced post-operative pain (WMD -1.27, 95% CI: -1.94 to -0.60, p < 0.001) on the VAS (0-10 scale). Significant reductions in anxiety levels were also observed. Patients receiving relaxation therapy required fewer analgesics. Effects were observed as early as the first post-operative day and persisted through hospital discharge.
Figures
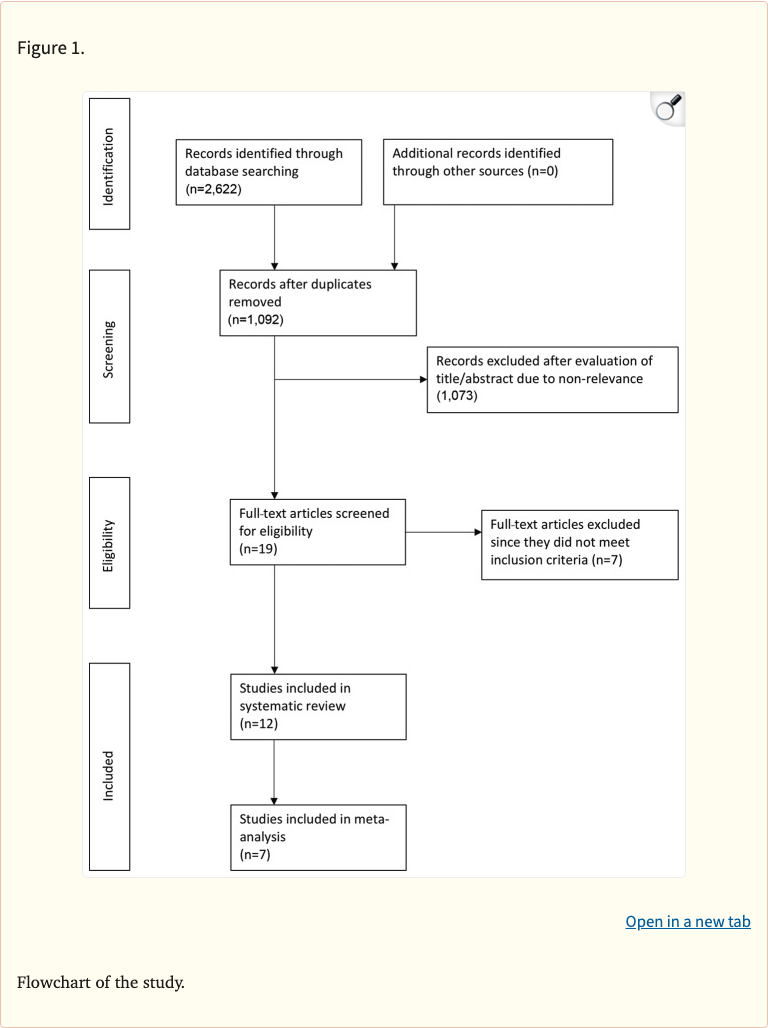 Figure 1
Figure 1
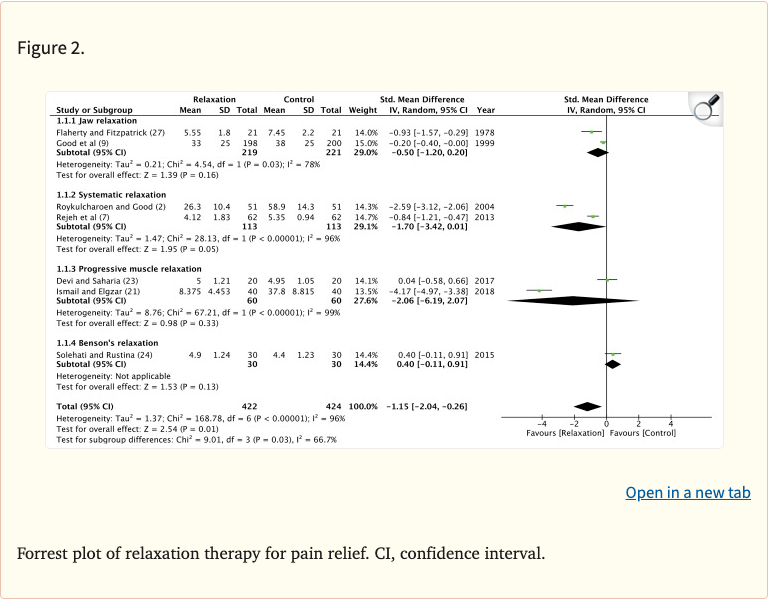 Figure 2
Figure 2
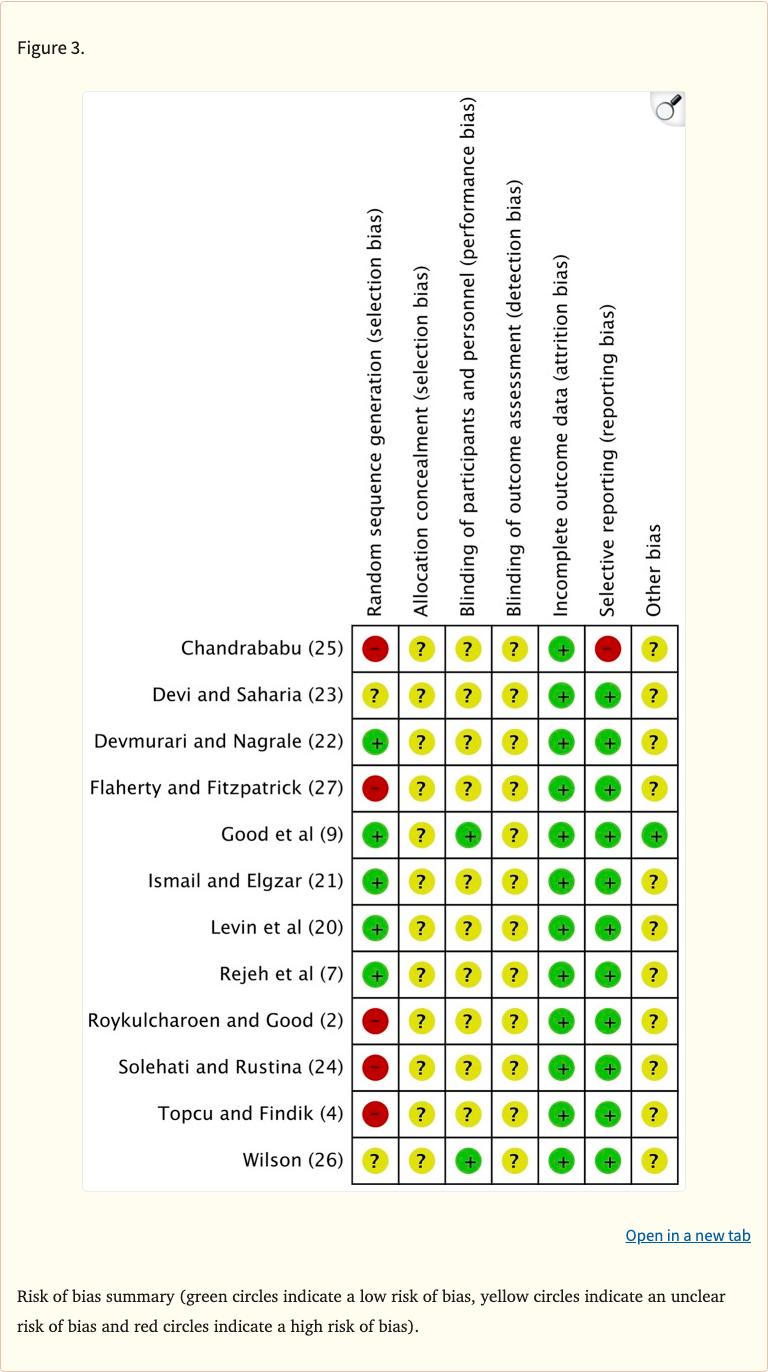 Figure 3
Figure 3
Limitations
Moderate heterogeneity across included studies. Relatively small number of included trials (11 RCTs). Variation in relaxation techniques used (PMR, jaw relaxation, guided imagery). Blinding of participants not possible due to the nature of the intervention. Most studies conducted in Asian populations, which may limit generalizability. Short follow-up periods limited to hospital stay.
