Key Takeaway
Dry needling significantly reduces neck pain immediately and short-term versus sham/placebo, and outperforms manual therapy at short-term follow-up.
Summary
This updated systematic review and meta-analysis evaluated the effectiveness of dry needling for myofascial trigger points associated with neck pain. The authors searched PubMed, CINAHL, Web of Science, and Cochrane databases through 2020 and identified 28 randomized controlled trials meeting inclusion criteria.
The meta-analysis compared dry needling against sham/placebo interventions, manual therapy, and other physical therapy treatments across immediate, short-term, and mid-term time points. The Cochrane risk of bias tool was used to assess study quality, and mean differences were calculated for pain intensity outcomes.
Results demonstrated that dry needling was superior to sham/placebo for reducing pain immediately (MD=-1.53 on a 10-point scale) and at short-term follow-up (MD=-2.31). Dry needling also outperformed manual therapy at short-term follow-up (MD=-0.51). However, no significant differences were found between dry needling and other physical therapy interventions, suggesting it is at least as effective as standard PT approaches for neck-related trigger point pain.
Methods
Systematic review and meta-analysis following PRISMA guidelines. Searched PubMed, CINAHL, Web of Science, and Cochrane Library databases. Included 28 RCTs evaluating dry needling for myofascial trigger points associated with neck pain. Assessed risk of bias using the Cochrane tool. Pooled mean differences for pain outcomes across immediate, short-term, and mid-term time points. Comparators included sham/placebo, manual therapy, and other physical therapy interventions.
Key Results
- Dry needling vs sham/placebo: significant pain reduction immediately (MD=-1.53) and short-term (MD=-2.31) on a 10-point scale
- Dry needling vs manual therapy: superior at short-term follow-up (MD=-0.51)
- Dry needling vs other physical therapy: no significant differences found
- 28 RCTs included with varying methodological quality
- Effects were consistent across immediate and short-term time points
Figures
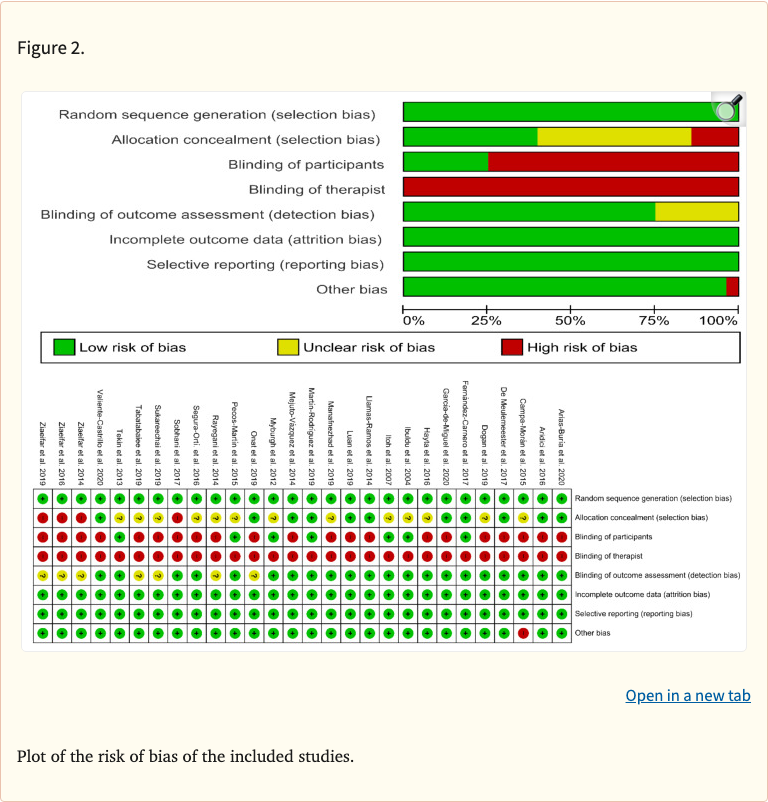 Figure 1
Figure 1
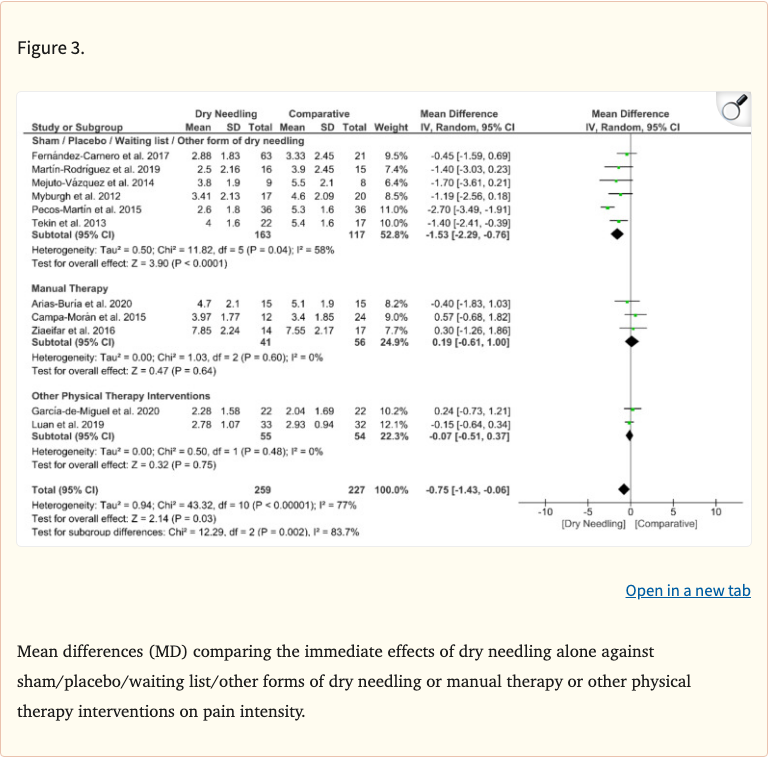 Figure 2
Figure 2
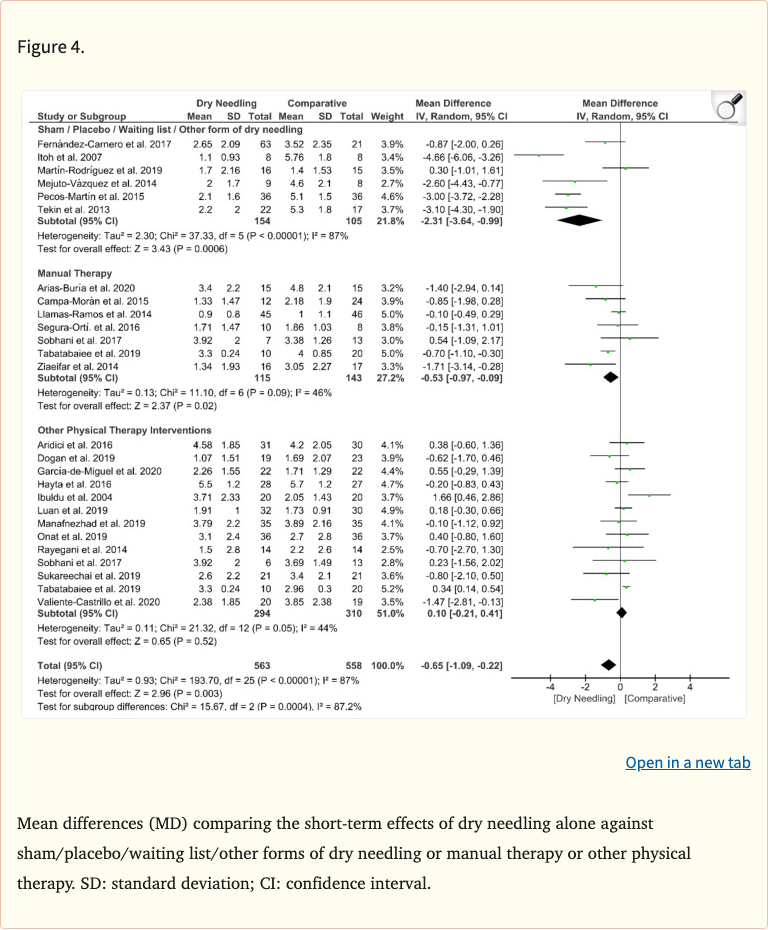 Figure 3
Figure 3
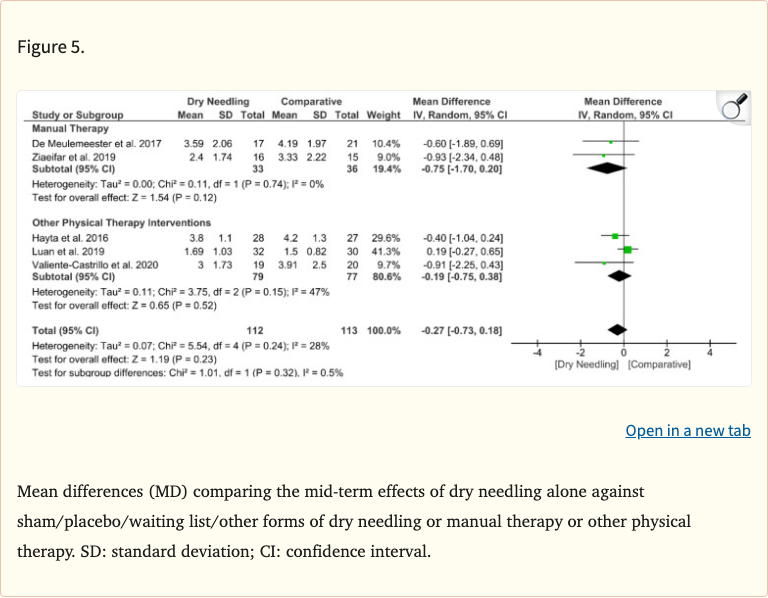 Figure 4
Figure 4
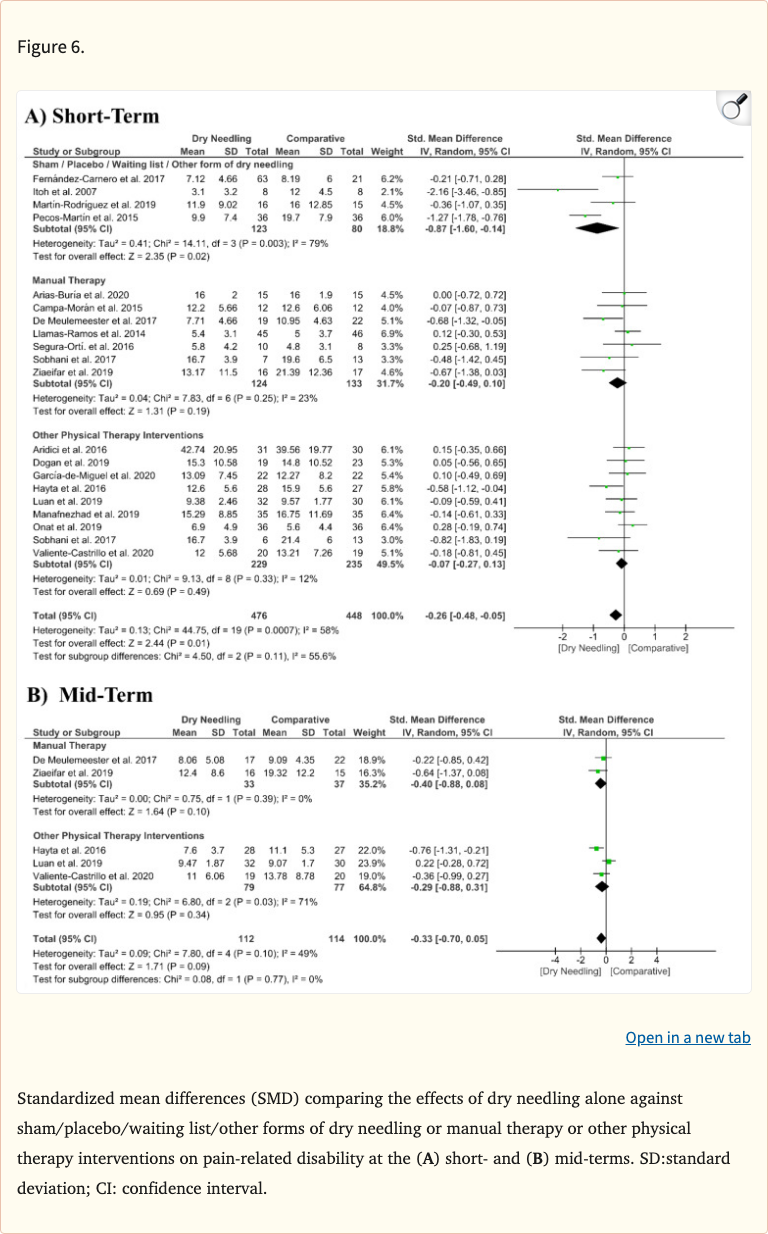 Figure 5
Figure 5
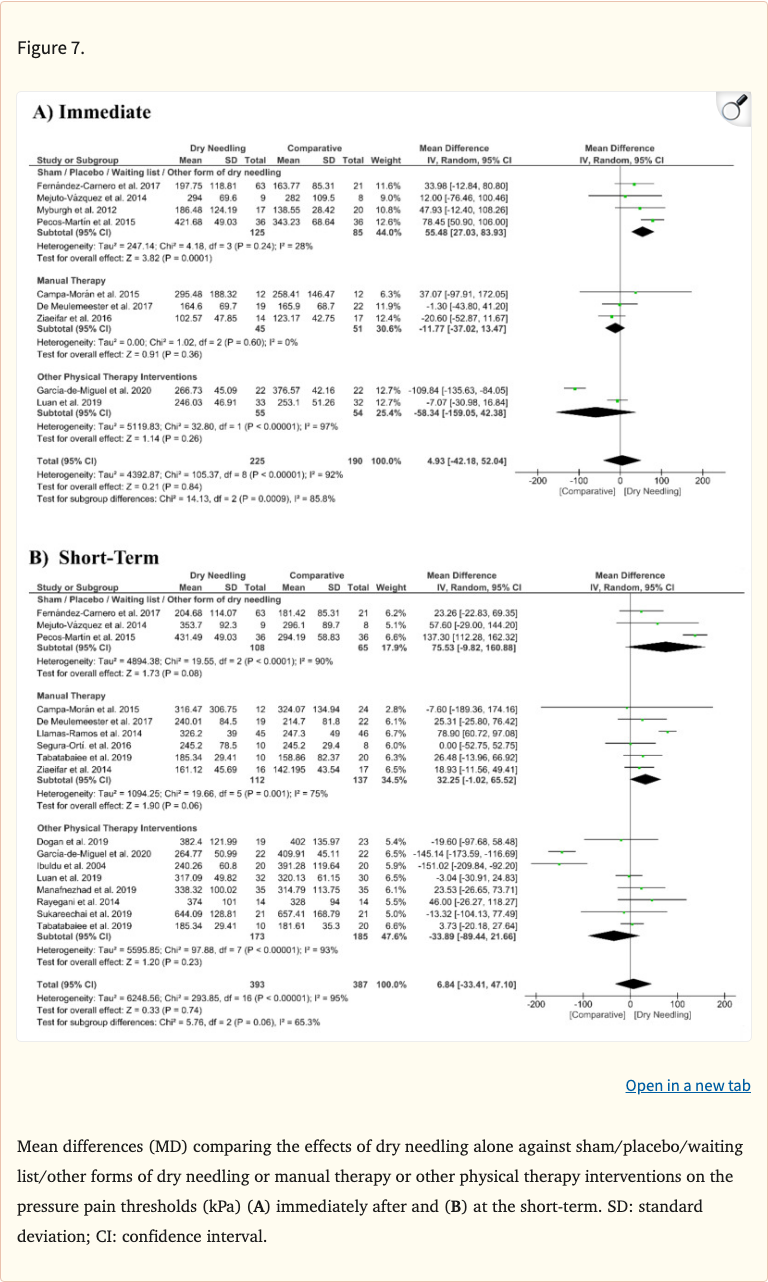 Figure 6
Figure 6
Limitations
- Heterogeneity across included trials in needling techniques, session frequency, and treatment duration
- Variable methodological quality among the 28 RCTs
- Limited data available for mid-term and long-term outcomes
- Most studies focused on pain intensity; fewer examined disability or quality of life
- Sham needling procedures varied across studies, which may affect blinding quality
