Key Takeaway
Triple-blind sham-controlled RCT found that photobiomodulation with red/NIR LEDs reduced ICU length of stay and improved muscle function in critically ill patients.
Summary
This randomized, triple-blind, sham-controlled trial investigated whether photobiomodulation (PBM) therapy using red and near-infrared LEDs could improve outcomes for critically ill patients in the intensive care unit. ICU-acquired weakness is a common complication that prolongs hospitalization and impairs recovery, making interventions that preserve muscle function highly valuable.
Patients in the PBM group received light therapy sessions targeting major muscle groups during their ICU stay, while the sham group received identical treatment with inactive devices. The triple-blind design ensured that patients, clinicians, and outcome assessors were all unaware of group assignments, providing a high level of rigor.
The results demonstrated that PBM therapy significantly reduced the length of ICU stay and improved muscle strength as measured by the Medical Research Council (MRC) scale. The PBM group also showed better functional outcomes at discharge compared to controls.
These findings suggest that photobiomodulation may be a safe, non-invasive adjunct therapy for preventing ICU-acquired weakness and accelerating recovery in critically ill patients, though larger multi-center trials are warranted to confirm these results.
Methods
Randomized, triple-blind, sham-controlled trial conducted in an ICU setting. Patients were randomly assigned to receive either active PBM therapy (red and near-infrared LEDs, wavelengths in the 630-850nm range) or sham treatment with identical-appearing but inactive devices. Treatment was applied to major muscle groups. Muscle function was assessed using the Medical Research Council (MRC) sum score. Primary outcome was ICU length of stay; secondary outcomes included muscle strength, functional status at discharge, and safety measures.
Key Results
- PBM group had significantly shorter ICU length of stay compared to sham group
- Muscle strength (MRC score) was significantly higher in the PBM group at discharge
- Functional outcomes at ICU discharge favored the PBM group
- No adverse events attributable to PBM therapy were reported
- Treatment compliance was high in both groups due to the passive nature of LED therapy
Figures
 Figure 1
Figure 1
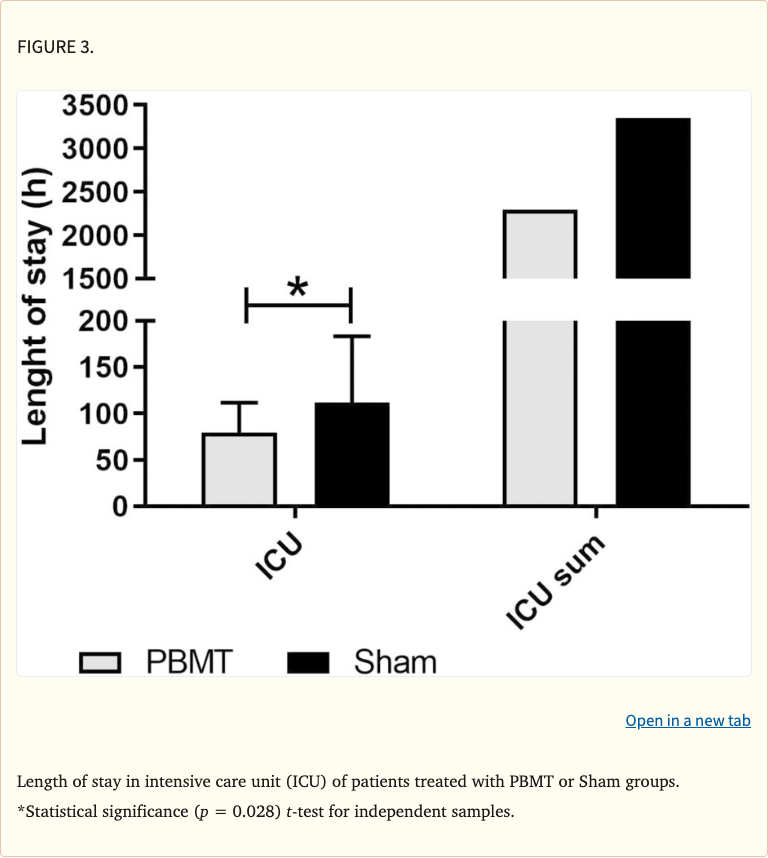 Figure 2
Figure 2
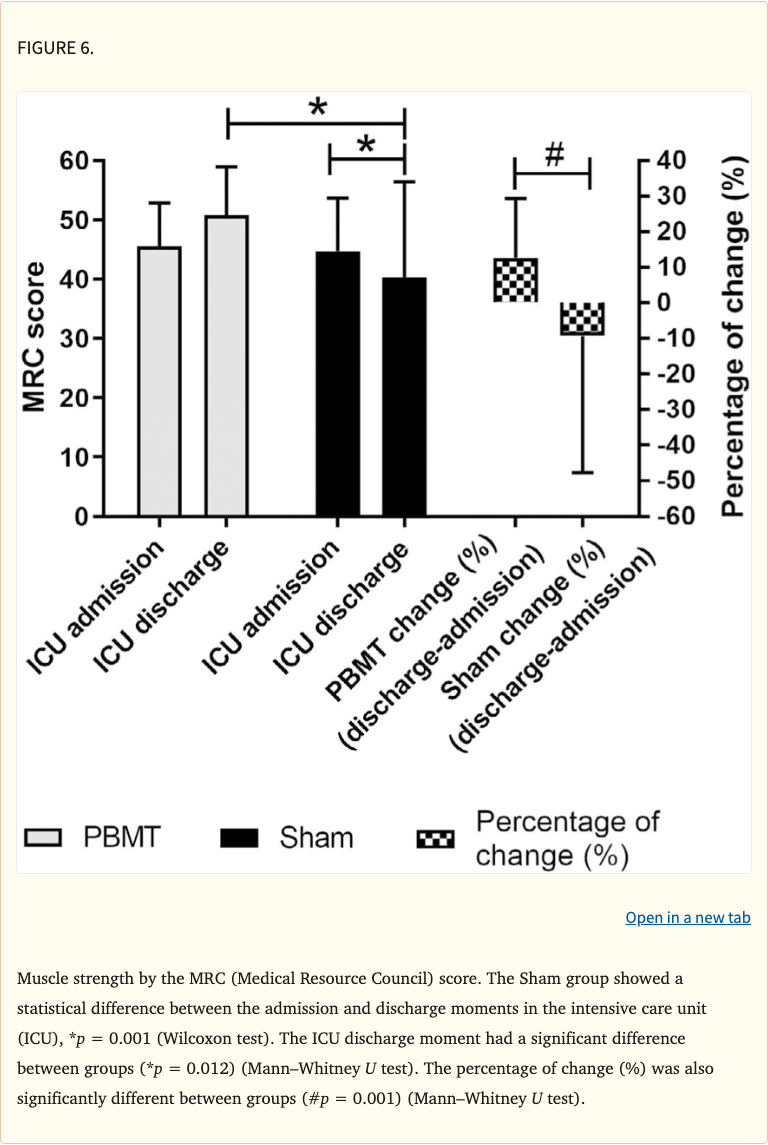 Figure 3
Figure 3
Limitations
- Single-center study limits generalizability
- Relatively small sample size
- ICU patient population may not generalize to healthy individuals or athletes
- Optimal dosing parameters (wavelength, power density, session duration) not fully explored
- Long-term follow-up beyond ICU discharge was limited
- Severity of illness at baseline may have varied between groups despite randomization
