Key Takeaway
Individual patient data meta-analysis of 20,827 patients confirmed acupuncture is effective for chronic pain, with effects persisting at 12-month follow-up and being clearly distinguishable from sham acupuncture
Summary
This landmark meta-analysis combined individual patient data from 39 high-quality RCTs to provide the most definitive evidence that acupuncture provides clinically meaningful pain relief beyond placebo effects. The analysis showed effects persist over time, strengthening the case for acupuncture as a legitimate treatment option for chronic pain conditions.
Methods
- Design: Individual patient data meta-analysis
- Patients: 20,827 from 39 RCTs
- Conditions: Musculoskeletal pain, headache, osteoarthritis
- Comparisons: Acupuncture vs sham, acupuncture vs no-acupuncture
- Follow-up: Extended analysis including 12-month outcomes
- Quality: Only high-quality trials included
Key Results
- Acupuncture superior to sham for all pain conditions:
- Effect size: 0.5 SD (moderate clinical significance)
- Musculoskeletal: Significant benefit
- Headache: Significant benefit
- Osteoarthritis: Significant benefit
- Acupuncture superior to no-acupuncture controls:
- Larger effect sizes than vs sham
- 12-month follow-up:
- 85% of pain reduction maintained
- Effects don't just fade after treatment stops
- Minimal heterogeneity across studies
- Effects consistent across different patient populations
Figures
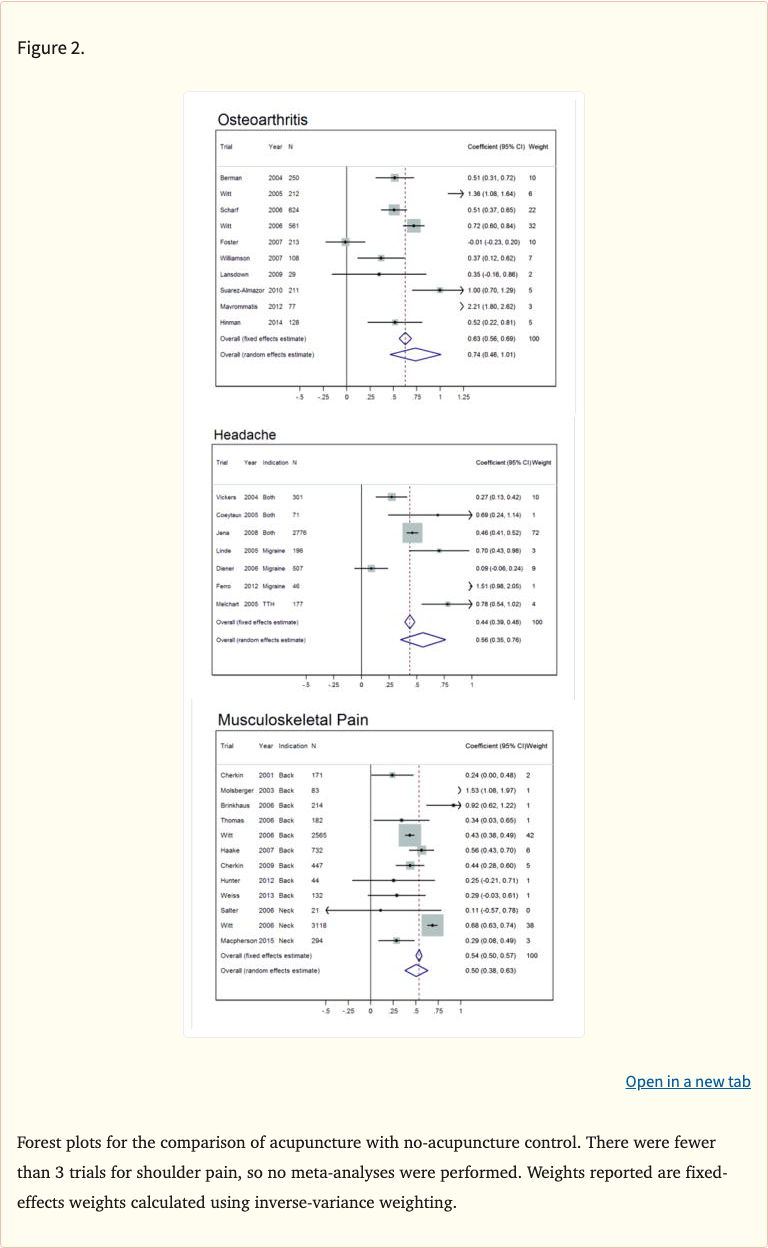 Figure 1
Figure 1
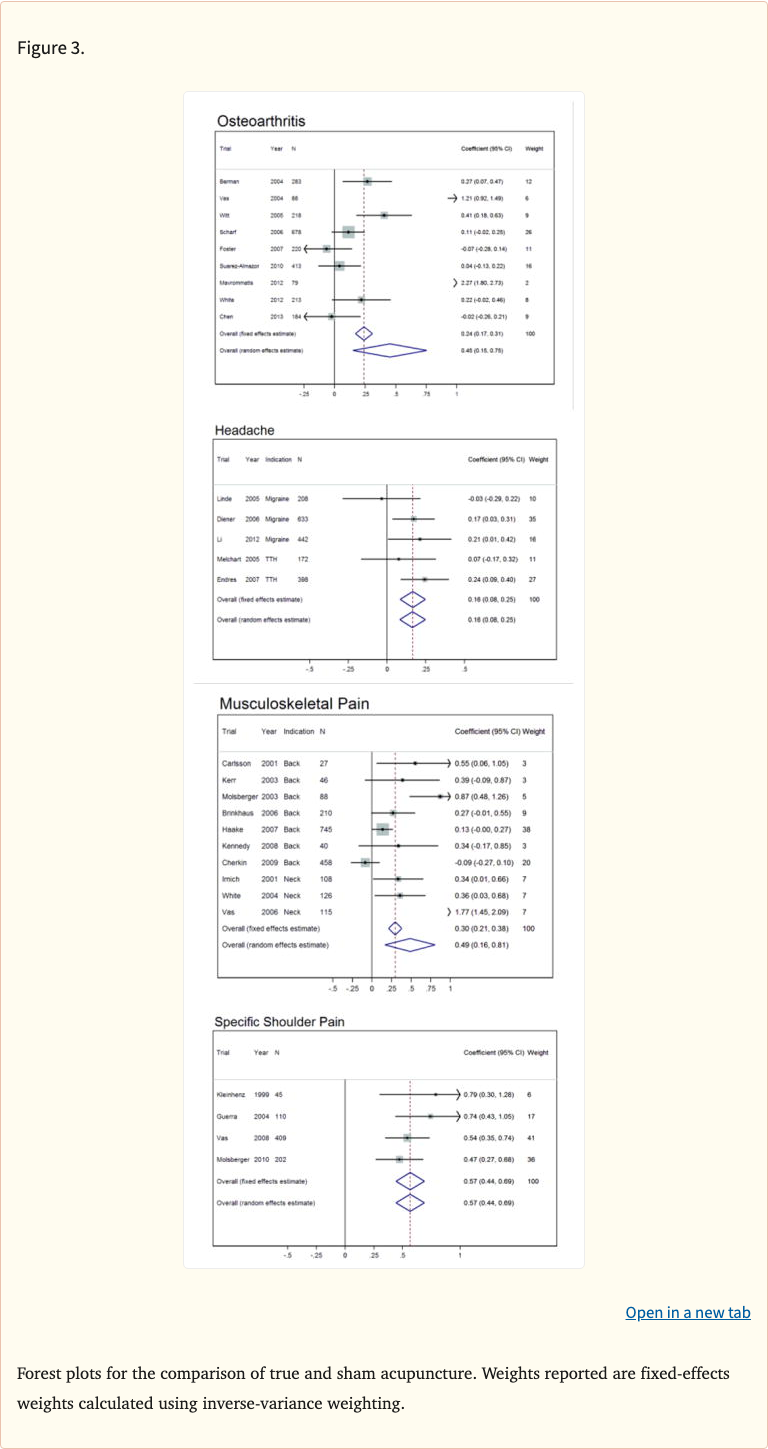 Figure 2
Figure 2
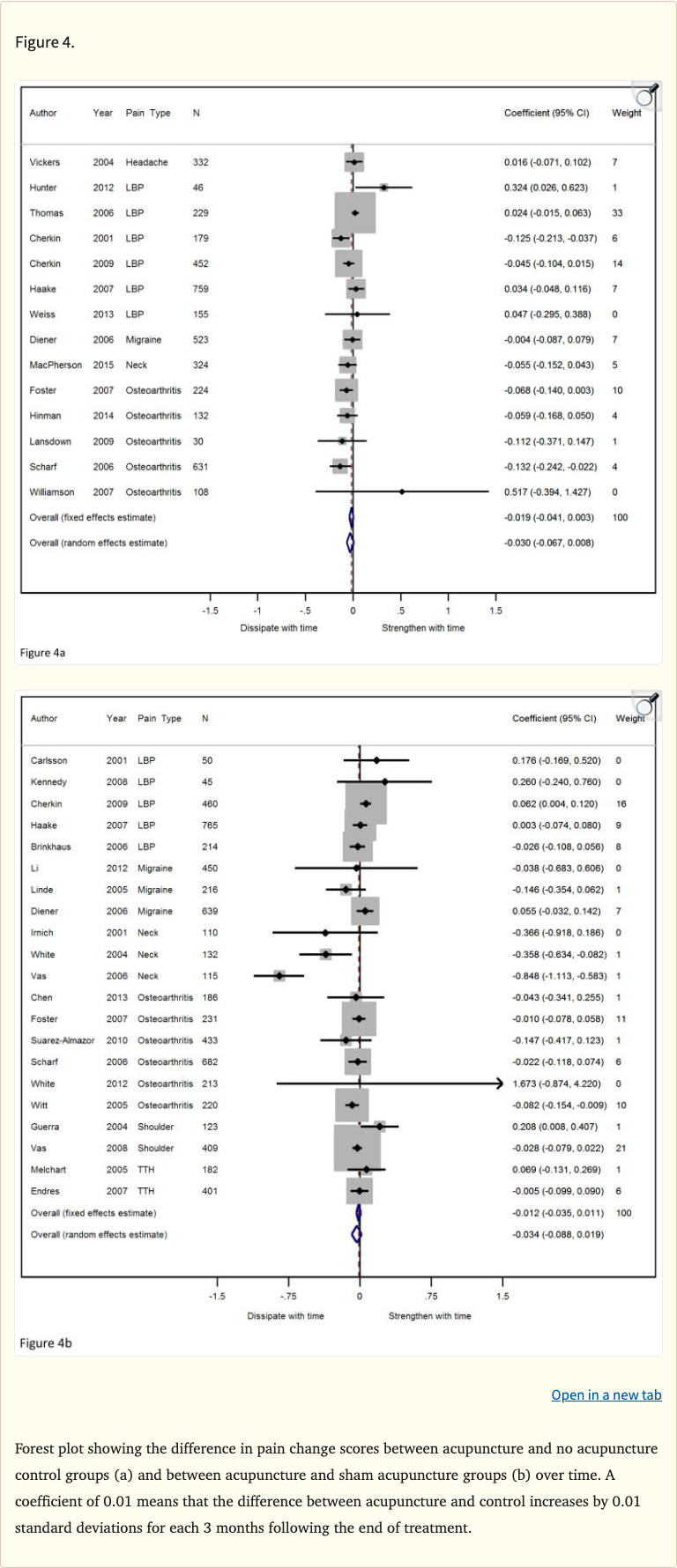 Figure 3
Figure 3
Limitations
- Sham acupuncture may not be true placebo (has physiological effects)
- Blinding imperfect in acupuncture trials
- Publication bias possible despite best efforts
- Effect sizes modest (but clinically meaningful)
- Optimal treatment protocols not established
