Key Takeaway
Meta-analysis of 7 RCTs (325 participants) found magnesium supplementation significantly reduces depression scores (SMD -0.92, p=0.001).
Summary
This systematic review and meta-analysis examined 7 randomized clinical trials with 325 adults (aged 20-60) diagnosed with depressive disorder. It assessed the effect of magnesium supplementation compared to placebo or control on depression severity.
Key findings:
- Significant reduction in depression scores with magnesium supplementation (SMD: -0.919, 95% CI: -1.443 to -0.396, p = 0.001)
- Benefits observed across different depression assessment scales
- Effect size was large, suggesting clinically meaningful improvement
Clinical implications:
Supports magnesium supplementation as a beneficial adjunct for depression management, though larger high-quality trials are needed to establish definitive clinical guidelines.
Methods
Systematic search of databases for randomized clinical trials comparing magnesium supplementation to placebo or control in adults with depressive disorder. Seven trials with 325 total participants were included. Depression outcomes were pooled using standardized mean difference (SMD).
Key Results
- Significant decline in depression scores with magnesium (SMD: -0.919, 95% CI: -1.443 to -0.396, p = 0.001)
- Large effect size indicating clinically meaningful improvement
- Consistent direction of effect across included trials
- Benefits observed in adults aged 20-60 with diagnosed depressive disorder
Figures
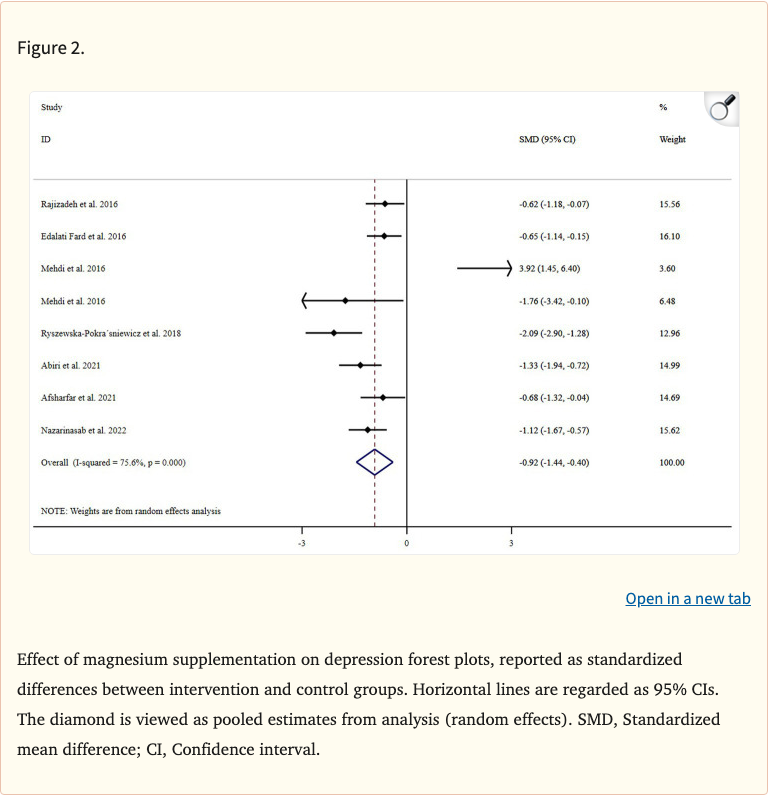 Figure 1
Figure 1
Limitations
- Small total sample size (325 participants across 7 trials)
- Moderate heterogeneity between studies
- Variable magnesium formulations, dosages, and treatment durations
- Need for larger, high-quality RCTs to confirm clinical applicability
