Key Takeaway
Tai Chi reduces fall odds by 53% in Parkinson's disease patients while significantly improving balance, functional reach, and mobility.
Summary
This meta-analysis evaluated the effects of Tai Chi exercise on fall prevention and balance performance in patients with Parkinson's disease (PD). Five randomized controlled trials with 355 PD patients were included, with evidence quality rated as moderate to high using the PEDro scale. Multiple databases were searched including PubMed, Cochrane Library, CINAHL, PEDro, Medline, and Embase.
The results demonstrated that Tai Chi significantly reduced fall odds by 53% (OR 0.47, 95% CI 0.30-0.74, p=0.001) compared to control groups. Balance improved meaningfully on the Berg Balance Scale (MD 3.47 points, p<0.001), functional reach increased (MD 3.55 cm, p<0.001), and mobility improved on the Timed Up and Go test (MD -1.06 seconds, p<0.001). All four outcome measures showed statistically significant benefits.
The authors conclude that Tai Chi is an effective physical training strategy for preventing falls and improving balance and functional mobility in people with Parkinson's disease. Given the progressive nature of PD and the high risk of falls in this population, Tai Chi offers a safe, accessible intervention that addresses multiple fall risk factors simultaneously.
Methods
- Systematic search of PubMed, Cochrane Library, CINAHL, PEDro, Medline, Embase, and other databases
- Included only randomized controlled trials of Tai Chi in Parkinson's disease patients
- 5 RCTs with 355 total PD patients analyzed
- Study quality assessed using PEDro scale (rated moderate to high)
- Outcome measures: fall rates, Berg Balance Scale, Functional Reach test, Timed Up and Go test
- Random effects meta-analysis with pooled effect estimates
Key Results
- Fall odds reduced: OR 0.47 (95% CI 0.30-0.74, p=0.001) - 53% reduction
- Berg Balance Scale improved: MD 3.47 points (95% CI 2.11-4.80, p<0.001)
- Functional Reach improved: MD 3.55 cm (95% CI 1.88-5.23, p<0.001)
- Timed Up and Go improved: MD -1.06 seconds (95% CI -1.61 to -0.51, p<0.001)
- All four outcome measures statistically significant
- Evidence quality rated moderate to high
Figures
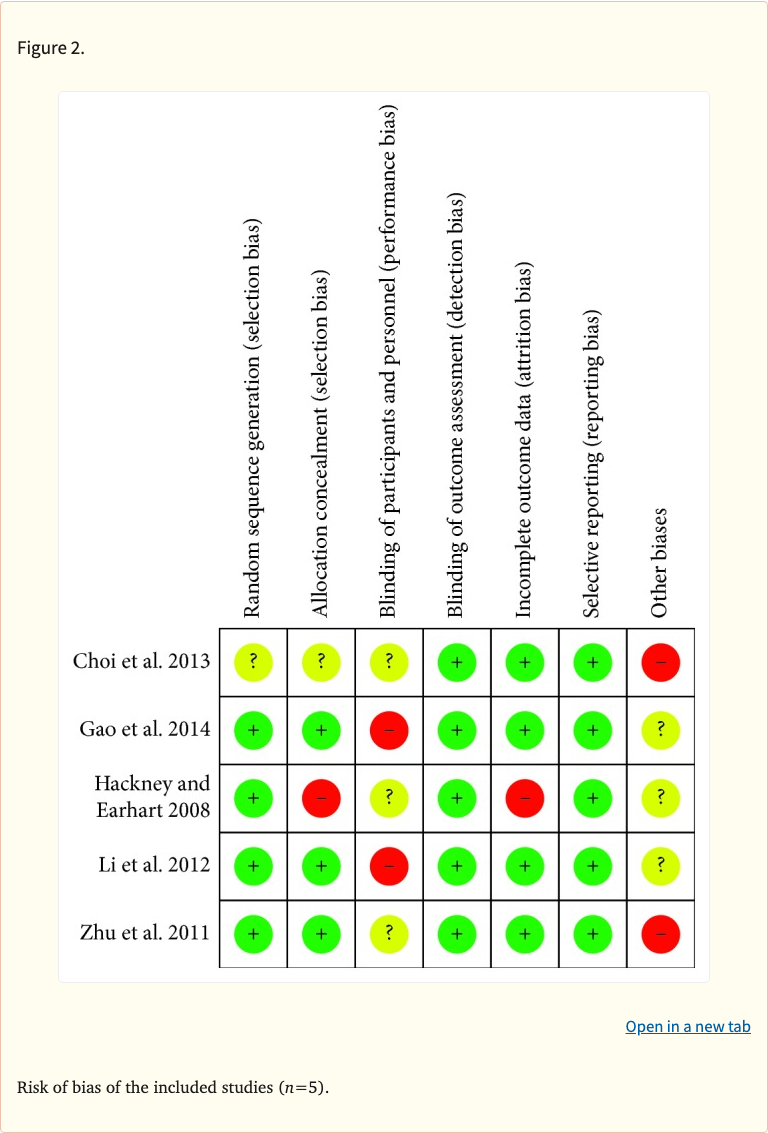 Figure 1
Figure 1
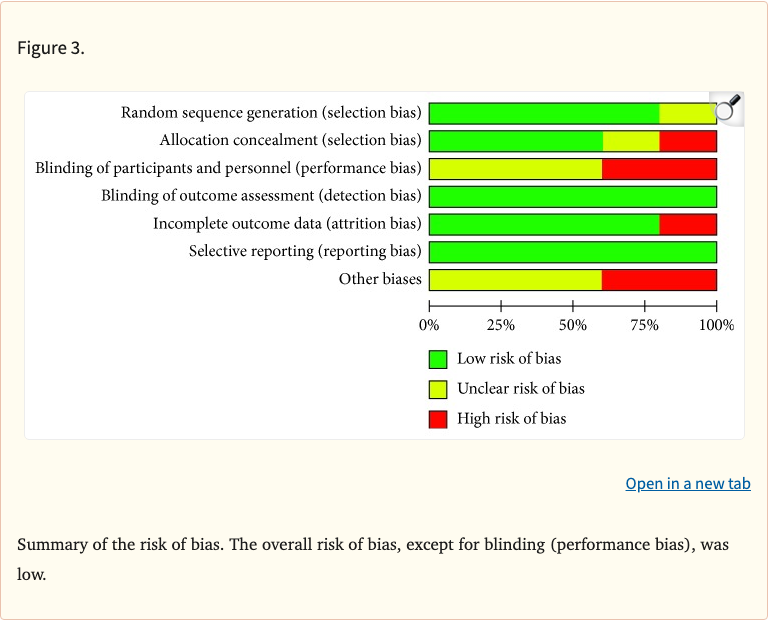 Figure 2
Figure 2
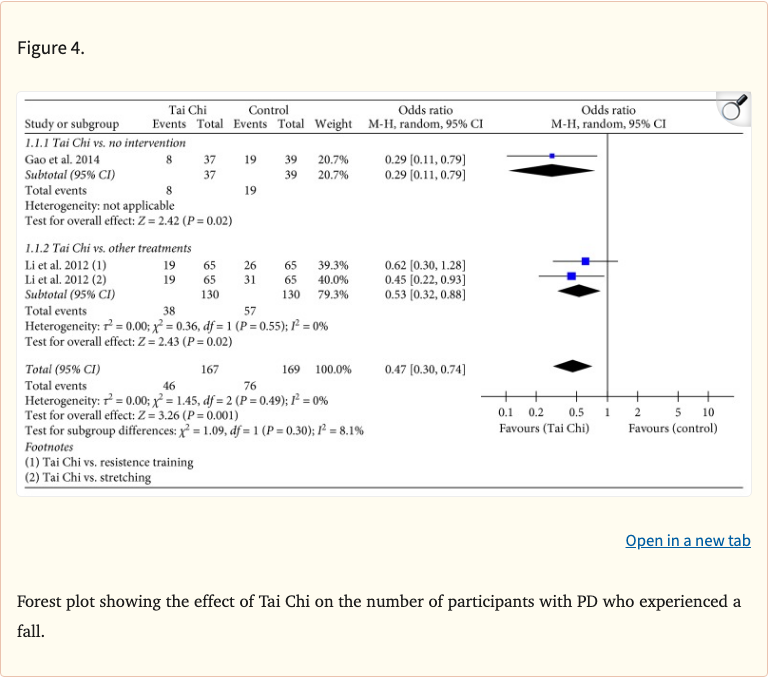 Figure 3
Figure 3
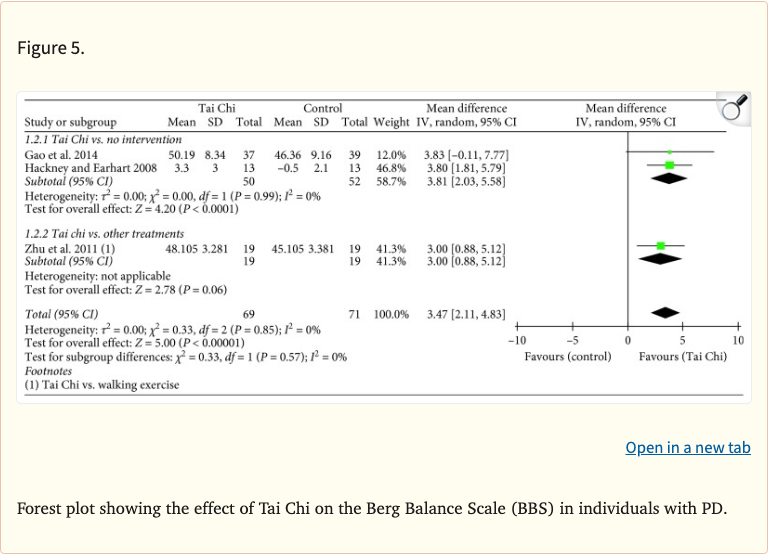 Figure 4
Figure 4
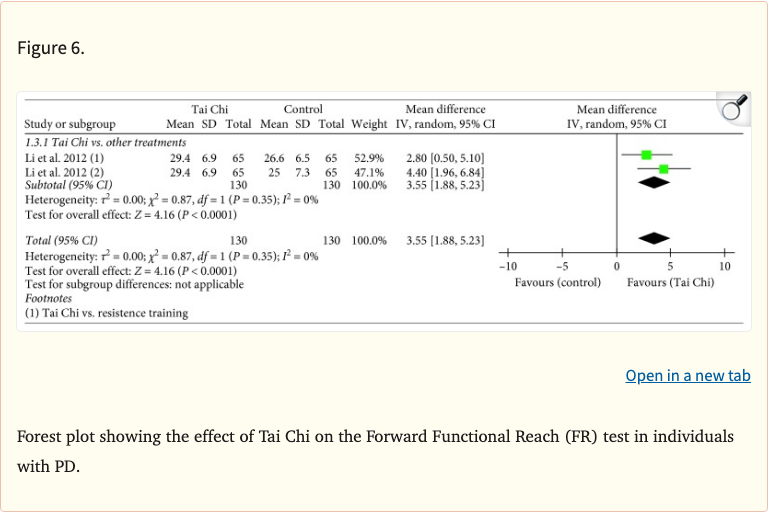 Figure 5
Figure 5
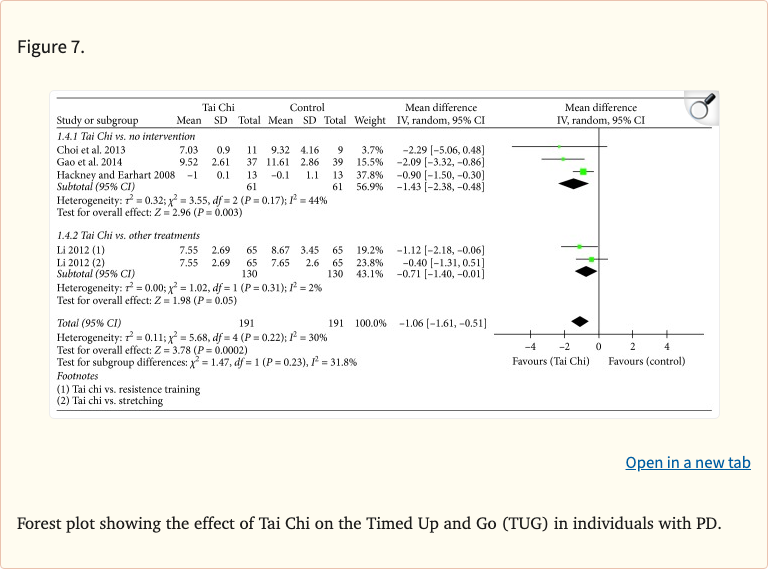 Figure 6
Figure 6
Limitations
- Small number of included trials (5 RCTs)
- Relatively small total sample size (355 patients)
- Heterogeneity in Tai Chi protocols across studies
- Most participants had mild-to-moderate PD, limiting applicability to advanced disease
- Limited follow-up duration in most trials
- Could not assess dose-response effects due to small number of studies
