Key Takeaway
Breathing re-education focusing on nasal breathing, slow breathing rate, and diaphragmatic activation addresses multiple OSA phenotypes and may reduce disease severity.
Summary
This review examines the role of breathing re-education as a therapeutic approach for obstructive sleep apnea (OSA), focusing on how it addresses the condition's multiple phenotypes and endotypes. The authors describe three core dimensions of breathing re-education: restoring nasal breathing, normalizing breathing volume and rate, and establishing diaphragmatic breathing patterns.
The paper outlines four key OSA phenotypes — anatomical compromise, high loop gain (unstable ventilatory control), low arousal threshold, and poor pharyngeal muscle responsiveness — and explains how breathing re-education can target each one. Nasal breathing reduces mouth breathing-related airway collapse, slower breathing rates improve ventilatory stability, and diaphragmatic breathing supports upper airway patency through improved tracheal tug mechanics.
The authors highlight that mouth breathing during sleep is a significant contributor to OSA severity and that interventions like myofunctional therapy and mouth taping can help restore nasal breathing. They also discuss the role of nitric oxide production in the nasal passages and its vasodilatory effects on the airways. The review concludes that breathing re-education represents a low-cost, non-invasive adjunct therapy that warrants further investigation through randomized controlled trials.
Methods
Narrative review of the literature examining breathing re-education techniques and their physiological mechanisms relevant to obstructive sleep apnea. The authors reviewed studies on nasal versus oral breathing, respiratory muscle training, myofunctional therapy, and the four-phenotype model of OSA. Evidence from clinical studies, physiological research, and mechanistic analyses was synthesized.
Key Results
The review found that nasal breathing produces nitric oxide which acts as a bronchodilator and vasodilator, improving airway patency. Mouth breathing during sleep was associated with increased airway collapsibility and higher AHI scores. Breathing re-education techniques targeting nasal breathing restoration, reduced breathing rate, and diaphragmatic activation showed promise across multiple OSA phenotypes. Myofunctional therapy exercises reduced AHI by approximately 50% in some referenced studies.
Figures
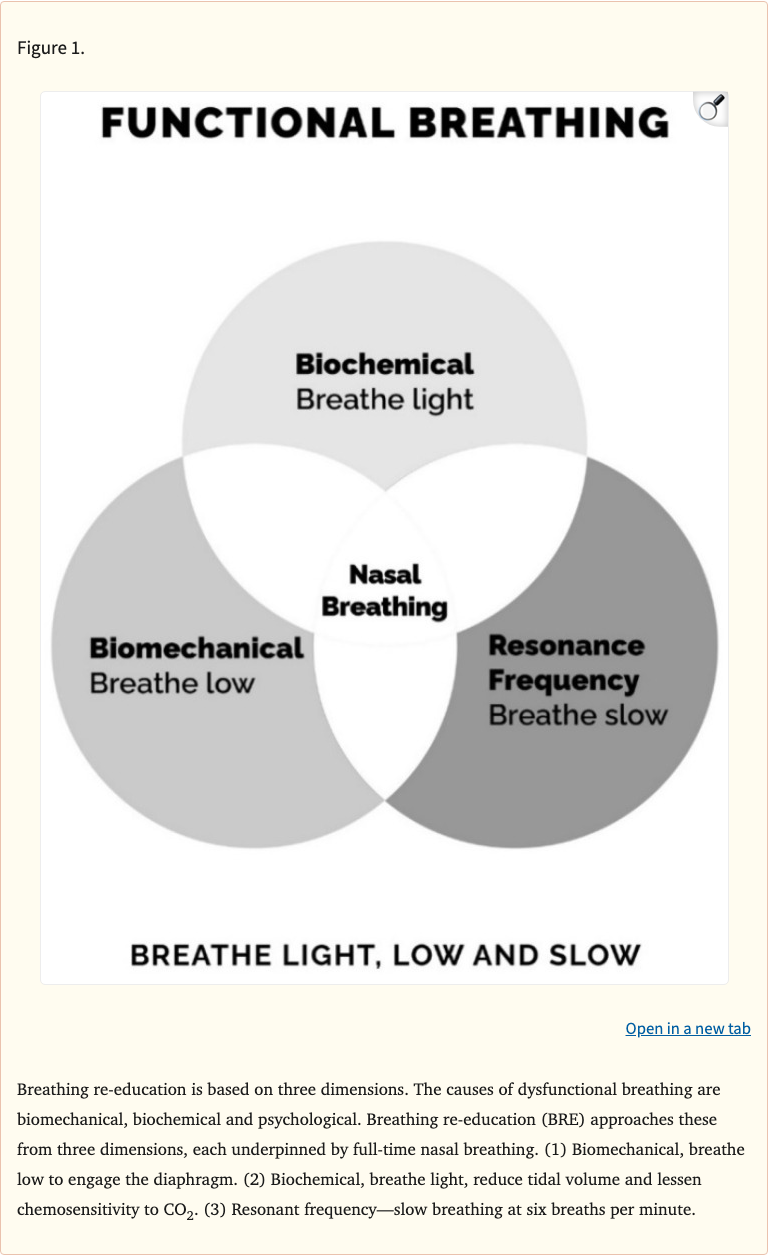 Figure 1
Figure 1
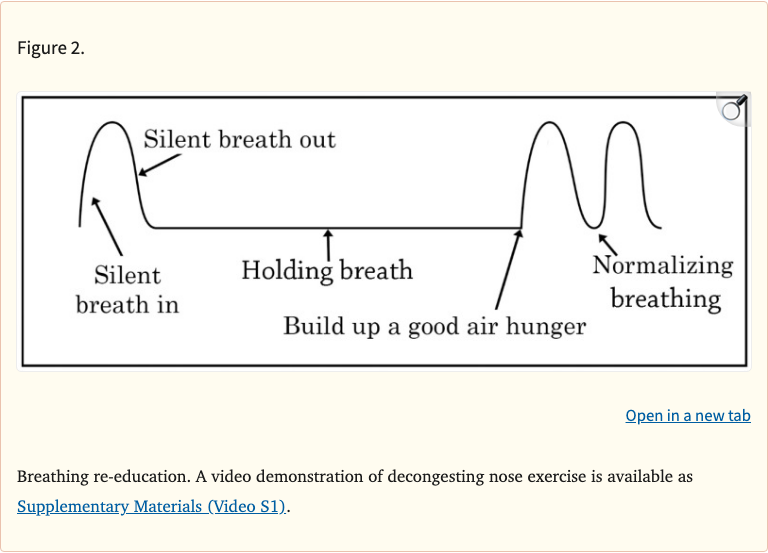 Figure 2
Figure 2
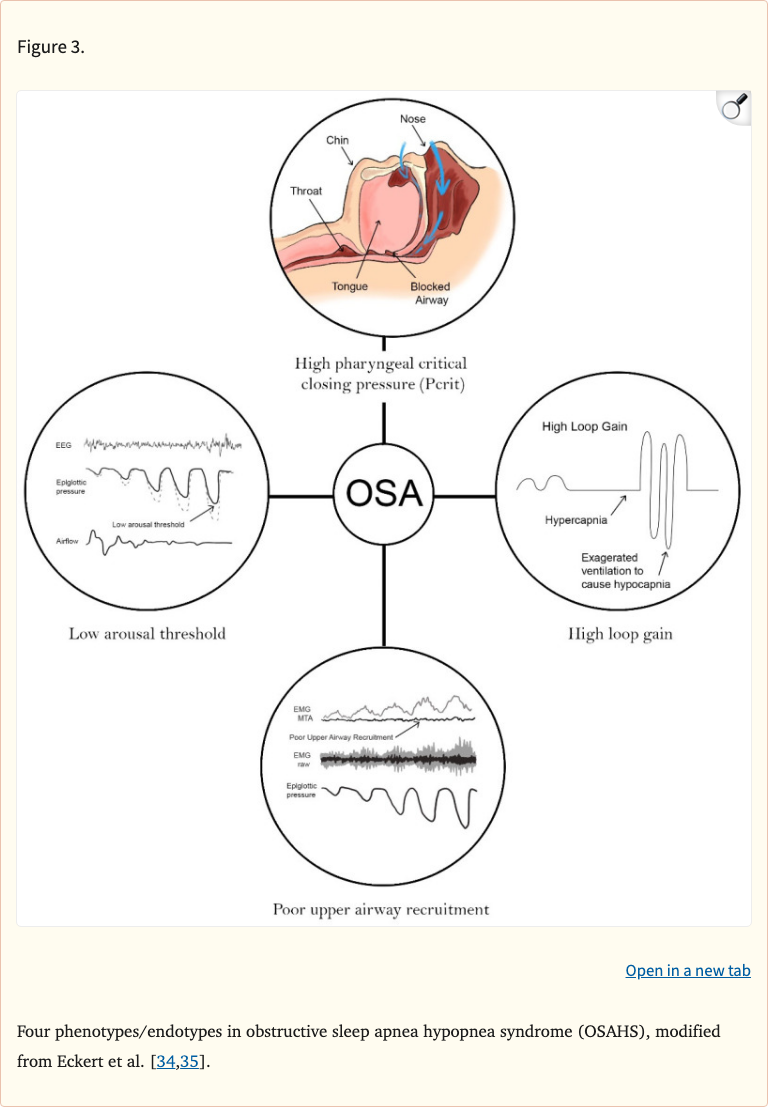 Figure 3
Figure 3
 Figure 4
Figure 4
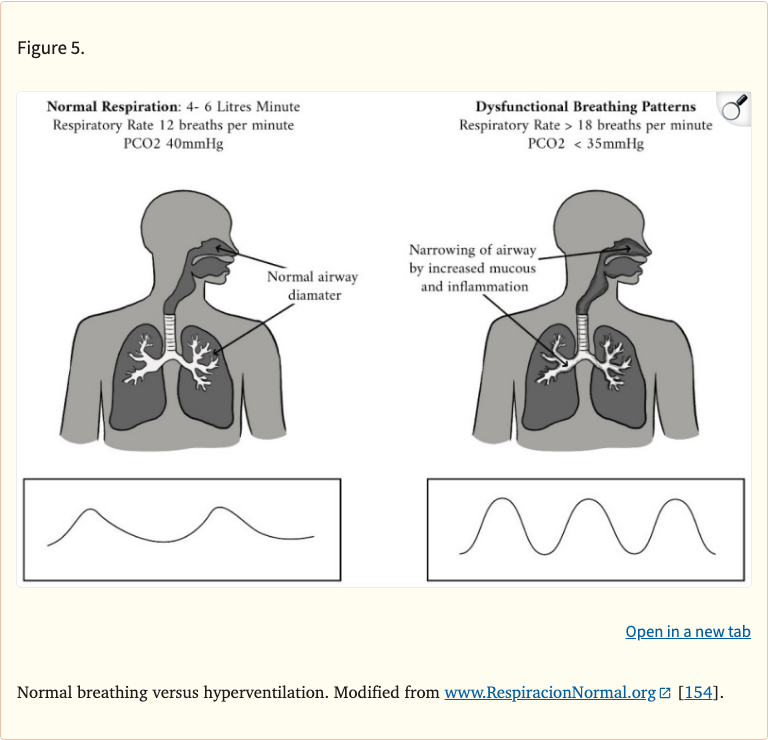 Figure 5
Figure 5
Limitations
As a narrative review, this paper does not provide a systematic assessment or quantitative synthesis of evidence. Many of the referenced interventions lack large-scale randomized controlled trials. The lead author has a commercial interest in breathing education products (Buteyko method), which represents a potential conflict of interest. The phenotype-based framework, while logical, has not been fully validated in prospective clinical trials.
