Key Takeaway
Prolonged fasting (48-72+ hours) triggers stem cell regeneration of the immune system through IGF-1/PKA pathway inhibition, potentially reversing immunosuppression.
Summary
This groundbreaking study from Valter Longo's USC lab demonstrated that prolonged fasting triggers regeneration of the immune system through stem cell activation. The research showed that fasting lowered IGF-1 and PKA signaling, which in turn promoted hematopoietic stem cell self-renewal.
The study found that cycles of prolonged fasting (48-72 hours in mice, equivalent to several days in humans) protected against chemotherapy-induced immunosuppression and promoted immune system regeneration. The mechanism involved killing old, damaged immune cells and triggering stem cells to create new ones.
This study provided mechanistic support for extended fasting as a potential intervention for immune system health and regeneration.
Methods
- Mouse models with various fasting durations
- Human subjects: Chemotherapy patients with fasting cycles
- Measured: IGF-1, PKA activity, stem cell markers
- Immune cell populations tracked
- Bone marrow analysis for stem cell activity
Key Results
- 48-72 hour fasting reduced IGF-1 and PKA levels
- Prolonged fasting killed damaged immune cells
- Stem cell regeneration triggered during refeeding
- Protection against chemotherapy-induced immunosuppression
- White blood cell counts restored faster with fasting
- Effects mediated by IGF-1/PKA pathway
Figures
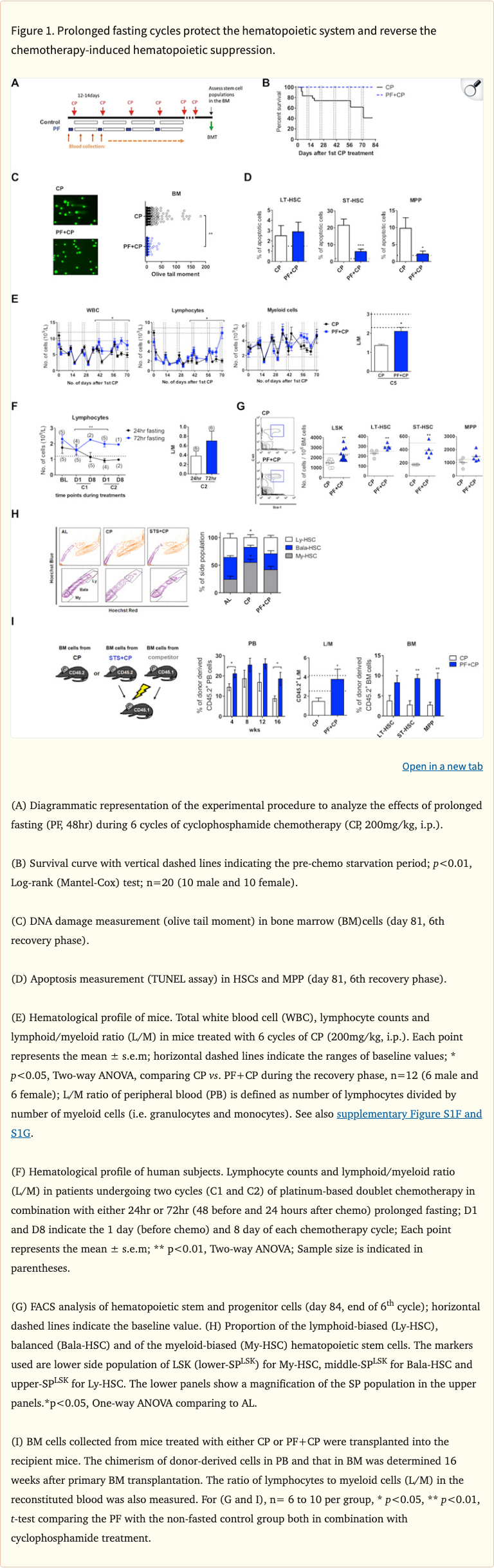 Figure 1
Figure 1
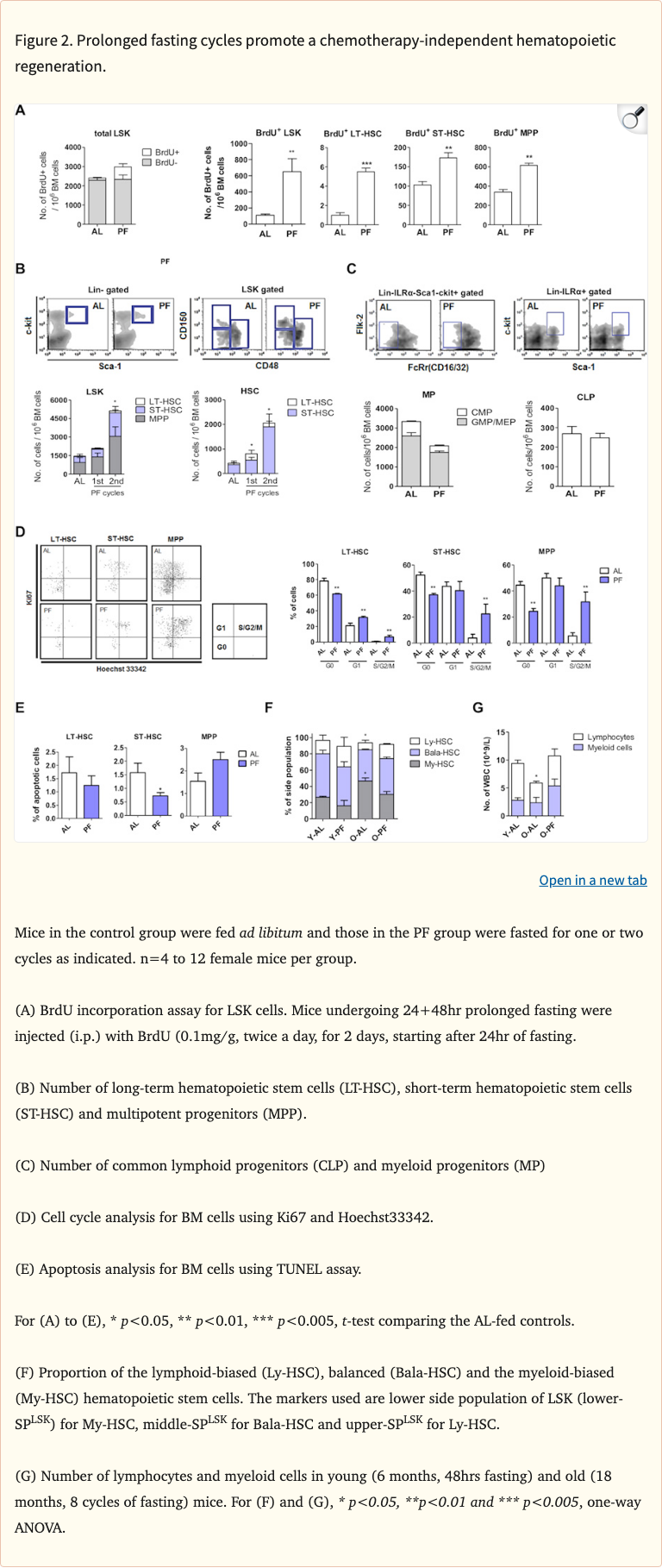 Figure 2
Figure 2
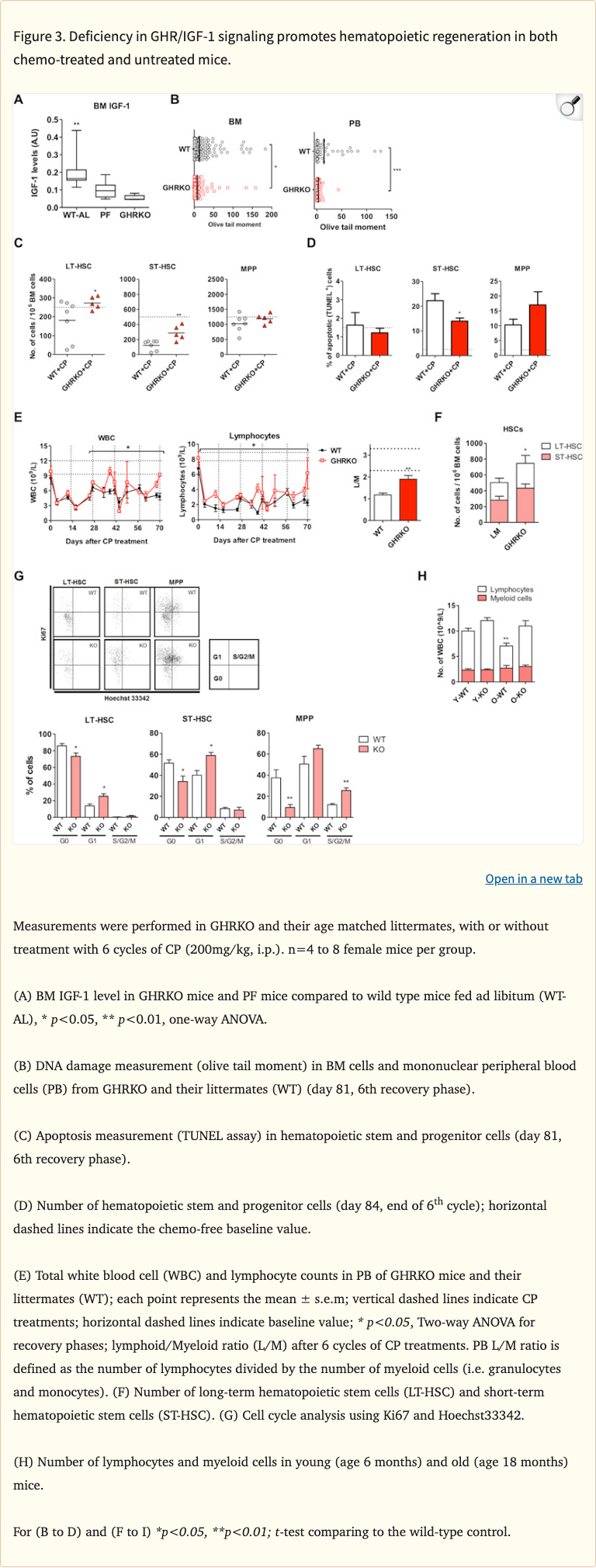 Figure 3
Figure 3
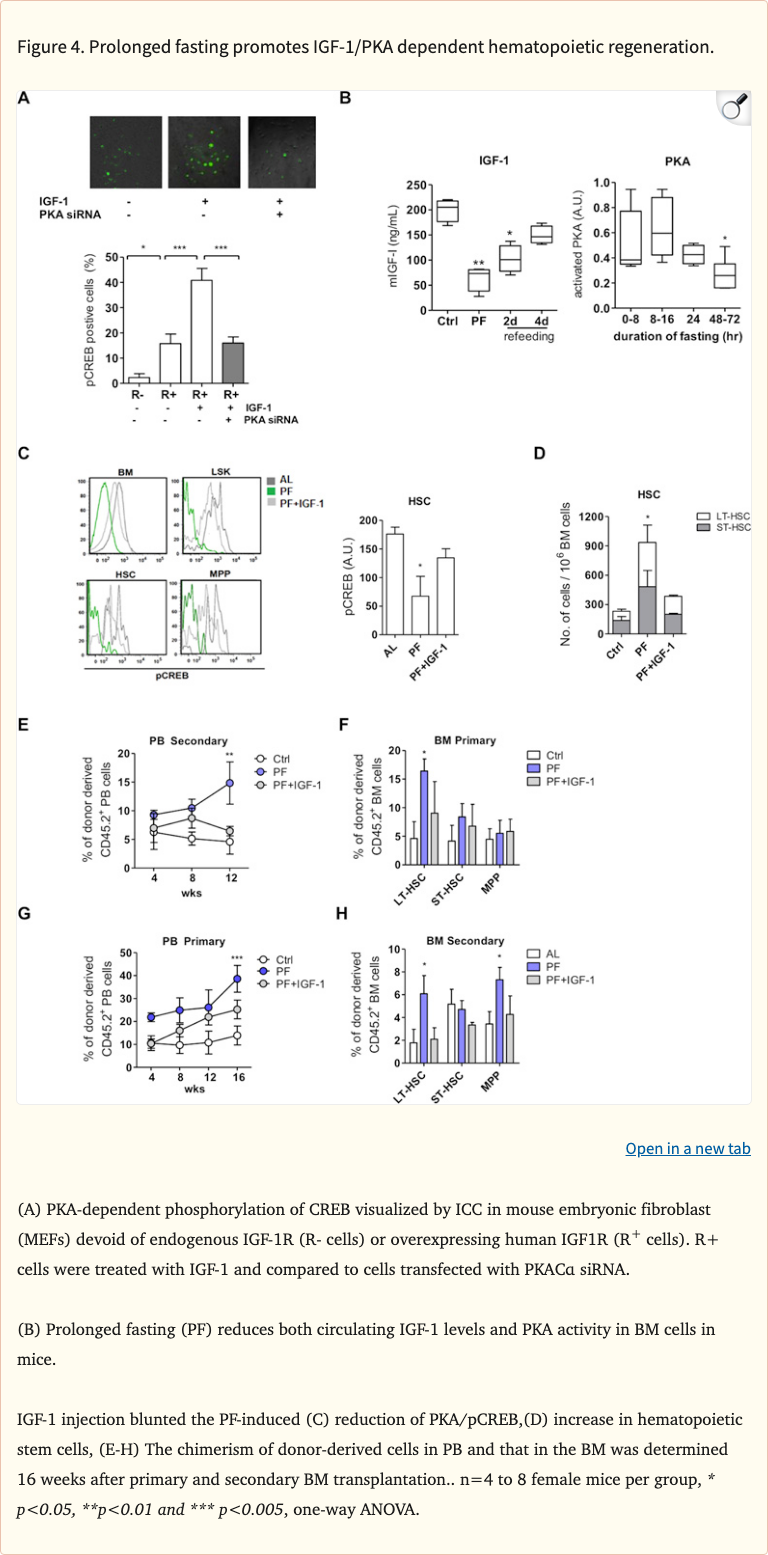 Figure 4
Figure 4
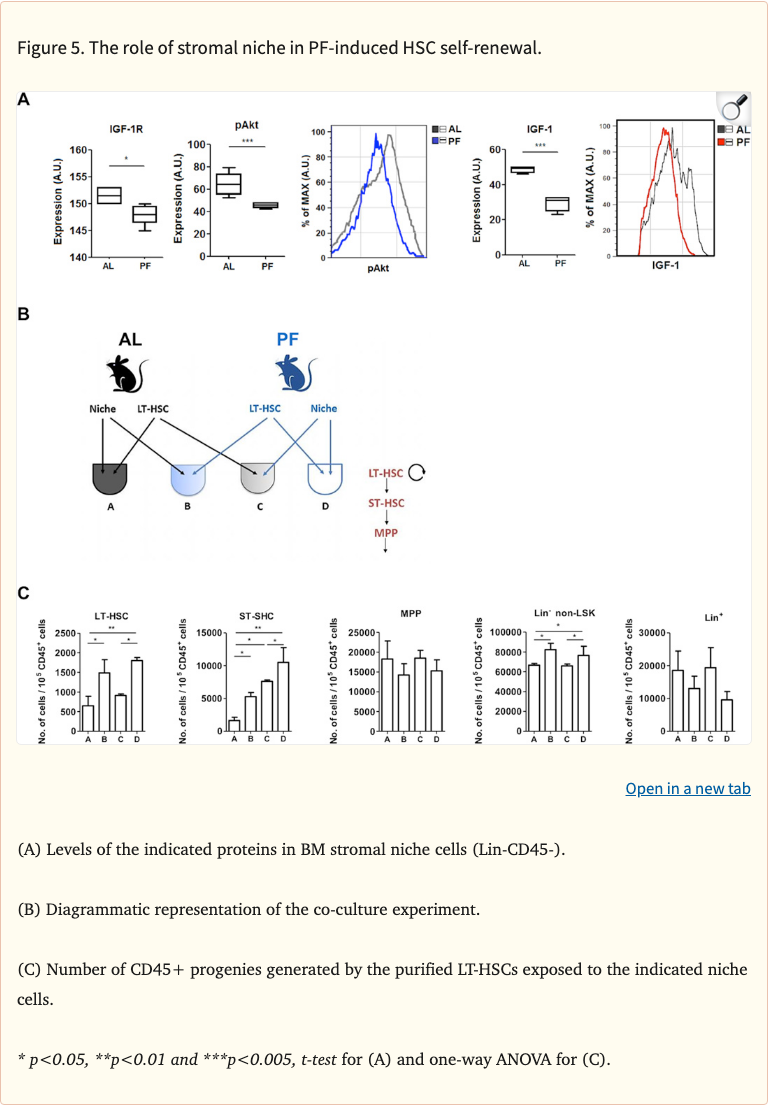 Figure 5
Figure 5
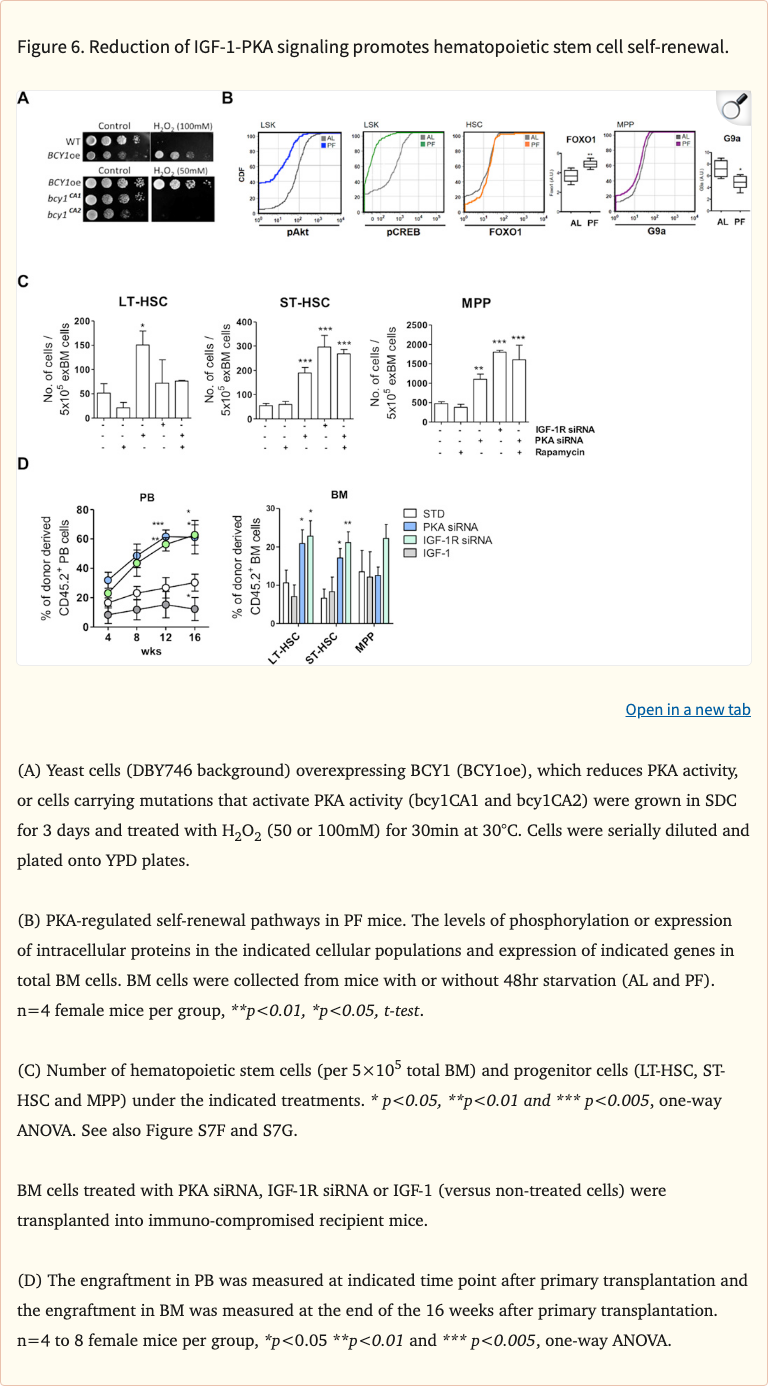 Figure 6
Figure 6
Limitations
- Primary findings in mice, limited human data
- Mechanism studies in animal models
- Human application requires further research
- Optimal fasting duration not established for humans
- Chemotherapy context may not generalize to healthy individuals
