Key Takeaway
IMT significantly improved inspiratory muscle strength (MIP +7.23 cmH2O) and reduced dyspnea in COPD patients, with sessions of 21-30 minutes at intensities above 50% MIP yielding the greatest benefits.
Summary
This systematic review and meta-analysis examined the effects of inspiratory muscle training (IMT) on respiratory function, exercise capacity, and quality of life in people with chronic obstructive pulmonary disease (COPD). The authors searched multiple databases and included 30 randomized controlled trials with a total of 1,578 participants.
The analysis found that IMT significantly improved maximal inspiratory pressure (MIP), a key measure of inspiratory muscle strength, with a weighted mean difference of 7.23 cmH2O. IMT also significantly reduced dyspnea scores, indicating meaningful improvements in breathing difficulty during daily activities. The review further explored how different training parameters — session duration, frequency, and intensity — modulated outcomes.
Subgroup analyses revealed that sessions lasting 21-30 minutes, conducted 5-7 times per week, and performed at intensities above 50% of maximal inspiratory pressure produced the most robust improvements. These findings provide practical guidance for clinicians designing IMT programs for COPD patients and reinforce the value of IMT as a complementary intervention alongside standard pulmonary rehabilitation.
Methods
Systematic review and meta-analysis of 30 RCTs (1,578 participants) identified from PubMed, Embase, Cochrane Library, and Web of Science. Studies compared IMT to sham training or no intervention in COPD patients. Subgroup analyses examined session duration, frequency, and intensity. Risk of bias was assessed using the Cochrane RoB 2 tool.
Key Results
IMT significantly improved MIP (WMD = 7.23 cmH2O, p < 0.05) and reduced dyspnea scores compared to controls. Sessions of 21-30 minutes produced larger MIP gains than shorter sessions. Training 5-7 times per week was more effective than lower frequencies. Intensities above 50% MIP yielded greater improvements than lower intensities. Effects on 6-minute walk distance and quality of life were not consistently significant across all subgroups.
Figures
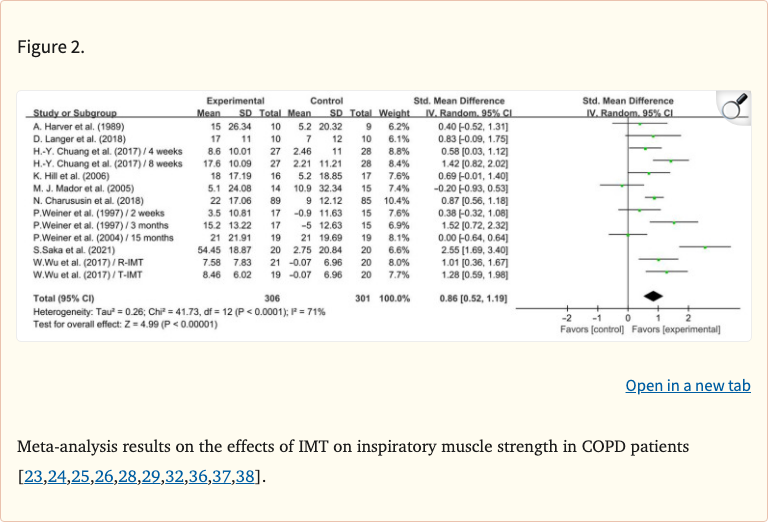 Figure 1
Figure 1
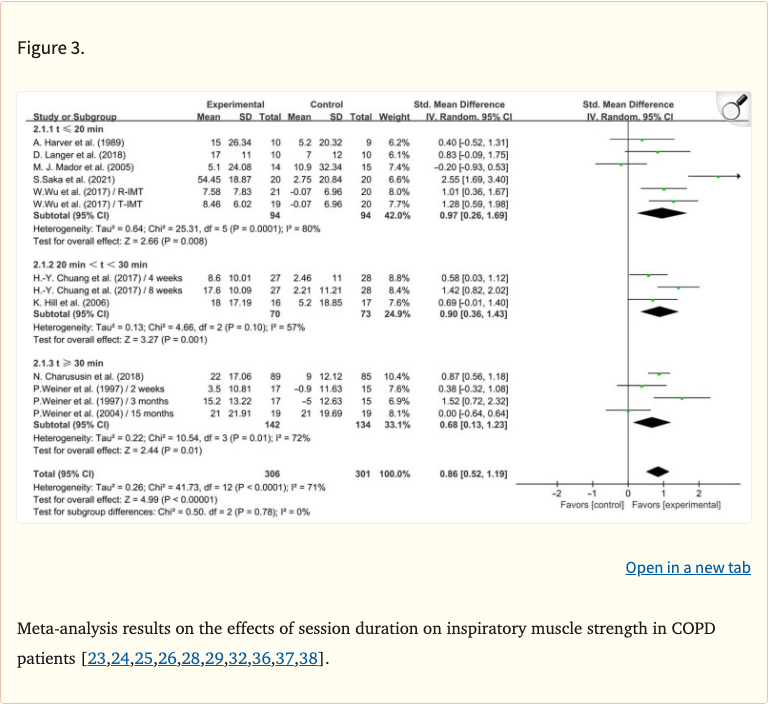 Figure 2
Figure 2
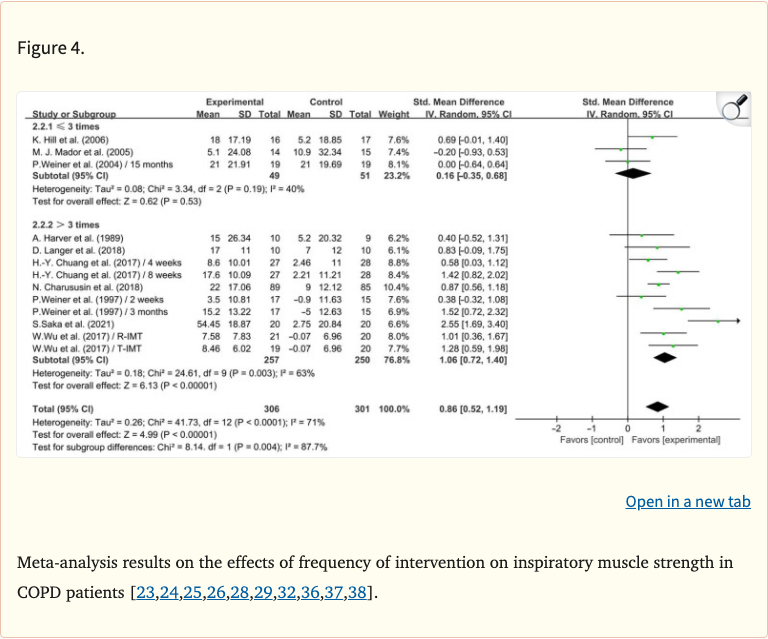 Figure 3
Figure 3
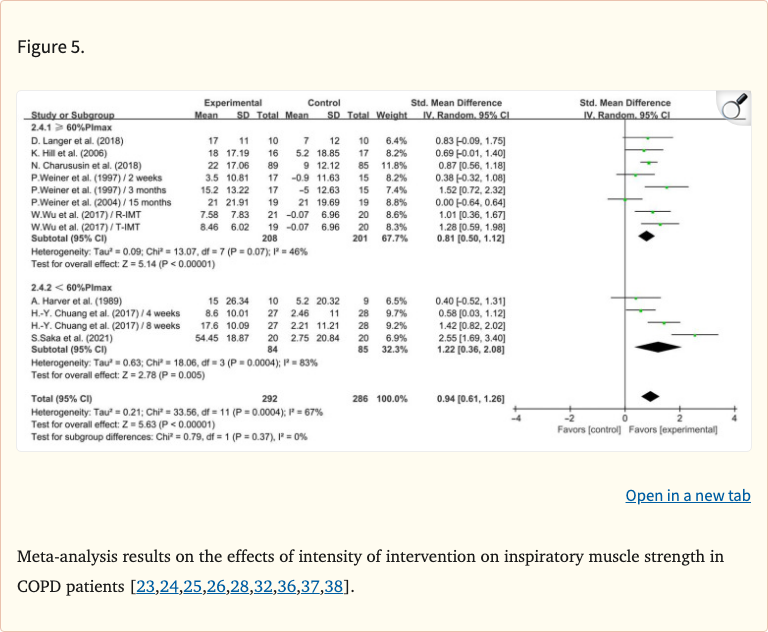 Figure 4
Figure 4
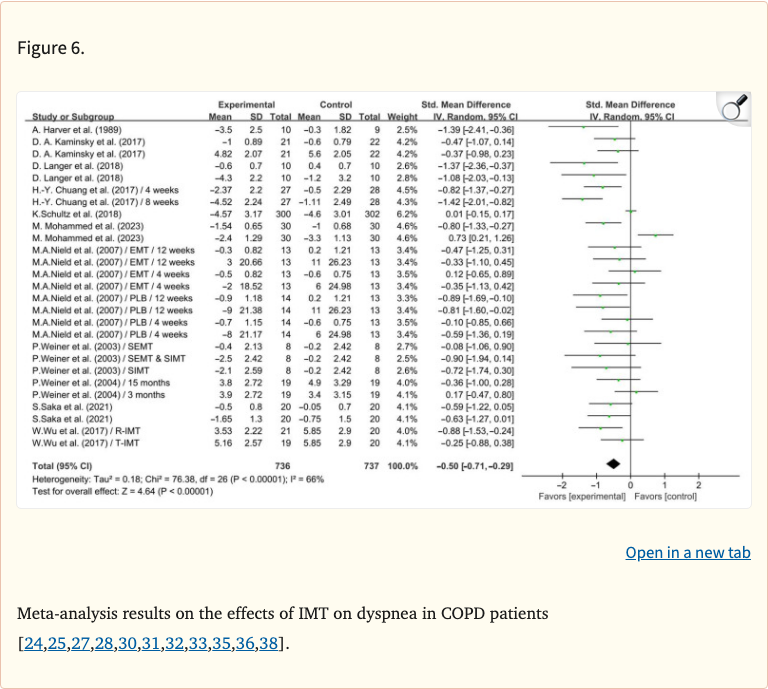 Figure 5
Figure 5
 Figure 6
Figure 6
Limitations
Significant heterogeneity among included studies in terms of IMT devices, training protocols, and outcome measures. Most studies had relatively small sample sizes. Some studies had unclear or high risk of bias. Long-term follow-up data were limited, making it difficult to assess sustained benefits. The analysis could not fully account for differences in COPD severity across studies.