Key Takeaway
Meta-analysis of 17 RCTs (889 participants) found magnesium supplementation significantly reduces CRP and increases nitric oxide levels.
Summary
This meta-analysis pooled 17 randomized controlled trials with 889 participants (mean age 46, 62.5% female) to assess the effect of oral magnesium supplementation on serum inflammatory markers compared to placebo.
Key findings:
- Magnesium significantly decreased serum C-reactive protein (CRP)
- Magnesium significantly increased nitric oxide (NO) levels
- Additional reductions observed in plasma fibrinogen, TNF-ligand superfamily member 13B, IL-1, and ST2 protein
- Trials had generally low risk of bias
Clinical implications:
These results support magnesium supplementation as a strategy for reducing systemic inflammation, with CRP and NO being the most robustly affected markers across studies.
Methods
Systematic search of multiple databases through November 2021. From 2,484 screened papers, 17 RCTs comparing oral magnesium supplementation to placebo were included. Outcomes were serum inflammatory markers. Risk of bias was assessed and found to be generally low.
Key Results
- Significant reduction in serum CRP levels with magnesium supplementation vs placebo
- Significant increase in nitric oxide (NO) levels
- Secondary reductions in plasma fibrinogen, tartrate-resistant acid phosphatase type 5, TNF-ligand superfamily member 13B, ST2 protein, and IL-1
- Effects were consistent across 17 trials with 889 total participants
Figures
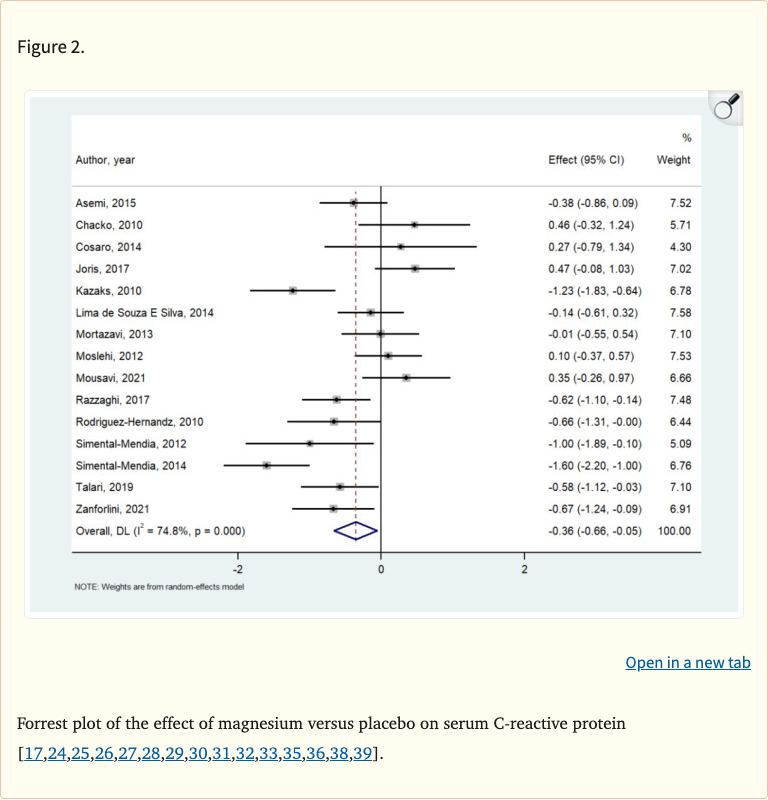 Figure 1
Figure 1
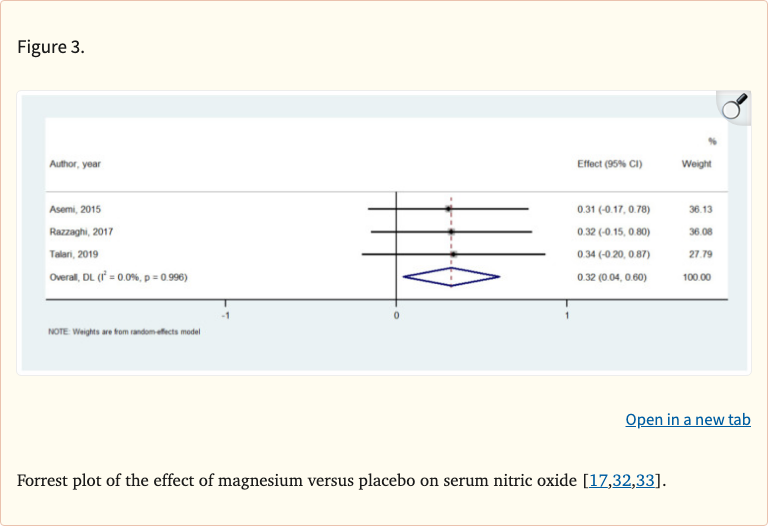 Figure 2
Figure 2
Limitations
- Heterogeneity in magnesium dosing, formulation, and duration across trials
- Relatively small total sample size (889 participants across 17 studies)
- Most participants were middle-aged females, limiting generalizability
- Inflammatory markers varied across studies, making some secondary outcomes less robust
